AI in Health care
AI in Medical Imaging: What is Coming Next

Speeds, accuracy, are vital for AI medical imaging. In case you do not know, one image can alter a diagnosis, or treatment. Artificial Intelligence will be big in healthcare, like it is in others. However, it won’t take the place of doctors, but make diagnosis and treatment faster.
AI in medical imaging is about pattern recognition at levels no human can achieve. These models analyze thousands of scans in just minutes. The result: radiology and diagnostic imaging get better clinical support.
This technology didn’t just arrive suddenly. Today, AI medical imaging products are used in hospitals, research facilities, and diagnostic laboratories globally.
Before delving deeper, let us see how AI works in medical imaging, the benefits it provides, and the future in healthcare.
What Is AI in Medical Imaging?
Artificial intelligence (AI) in medical imaging is a term that applies to a computer system that interprets the images based on the patterns it has ‘seen’ before.
These are based on machine learning and deep learning models trained on extensive datasets of labeled medical images. The system they create is more accurate after exposure to more data for the models.
Convolutional neural networks are what the majority of medical imaging AI depend on. They are very useful in image analysis, detecting edges, shapes, textures, and spatial relations. This allows AI to detect abnormalities at high precision, such as tumors, fractures, or damaged organs.
AI does not view images the way a human does. It transforms images into numbers and looks at pixel-level patterns. That’s the sort of difference that allows AI to recognize changes that are visually undetectable but important.
The output of the AI imaging system comprises classifications, probability scores, segmentation maps, and alerts. These outputs help during diagnosis, reporting, and treatment planning.
Why Medical Imaging Needs AI Support
Medical imaging demand is increasing by the day. CT scans, MRIs, X-rays, and ultrasounds are constantly imported. AI in radiology helps reduce workload by highlighting urgent cases and inaccurate research.
Human interpretations differ with experience, workload, and environmental conditions. AI offers homogeneous analysis, which is the same over time and across institutions. This uniformity is useful in the larger healthcare systems.
Technologies Behind AI in Medical Imaging
Deep learning is the basis of the majority of imaging AI solutions. These models depend on having large, interpreted datasets. The quality of data is as important as the quantity in medical image analysis.
Training datasets often contain images from different machines, patient groups, and types of clinical settings. This variation allows models to better generalize to unseen, real-world settings.
Computer vision techniques enable the AI to point out where an abnormality lies within images. For instance, segmentation algorithms delineate tumors or organs, enable physicians to quantify size, shape, and changes.
Machine learning models also integrate imaging data with clinical data. This fusion increases diagnostic confidence by providing context beyond the image alone.
Applications of AI in X-Ray Imaging
X-ray imaging is among the first domains where AI demonstrated clinical service. Chest X-rays are used routinely in diagnosing pneumonia, tuberculosis, fractures, and lung nodules.
Systems for reading AI medical imaging can interpret chest X-rays in seconds. They detect disease-associated patterns and produce probability scores, which can be used as a second opinion for radiologists in the interpretation.
Research shows that AI improves detection rates for e.g., lung nodules and pneumothorax. In emergency medicine, this can make a big difference in patient outcomes. AI is now bolstering screening programs in regions where radiology expertise is scarce. This use case expands access to diagnostic care for populations in need.
AI in CT Scan Analysis
CT scanning generates a massive amount of data. A CT scan may include hundreds of slices, and meticulously reviewing each one is a time-consuming process. These sequences are assessed in parallel by AI CT scan applications. They recognized anomalies, such as internal bleeding, pulmonary embolism, and tumors.
AI is essential in stroke care. Automated systems identify large vessel occlusions and notify the clinical team instantly. This pace decreases treatment latencies and enhances survival rates.
Also in CT imaging, AI is being explored for quantitative analysis to more accurately track the progression of disease and response to treatment.
AI in MRI Reading
MRI offers excellent soft tissue imaging, but takes more time to acquire and interpret. AI streamlines the two. Reconstruction capabilities of AI MRI solutions to address this, shortening the scan time while preserving image quality. Faster scans enhance patient comfort and throughput.
When it comes to interpretation, AI detects abnormalities in the brain, spine, joints, and organs. It aids the diagnosis of diseases such as multiple sclerosis, brain tumors, and ligament injuries. These tools increase precision and reduce reader variability, notably in challenging cases.
AI In Ultrasound Imaging
Operator dependence is strong in ultrasound imaging. The quality of images or interpretation can differ quite a bit from user to user. AI-controlled ultrasound devices to assist in image acquisition. They instruct users to hold probes at the right angle(s) to obtain diagnostic images.
Moreover, AI enables expanded ultrasound applications in primary care and in field locations, where specialist availability is limited.
The AI Revolution in Radiology
The application of AI in radiology is not confined to image reading. It is a resource for imaging job flows during the lifecycle. AI software triages incoming cases and prioritizes critical findings. That raises this urgent case priority immediately, which is great.
Measurements are extracted, and structured reports are populated using automated reporting solutions. This standardization streamlines the reporting process and saves time.
Quality control: AI is also used to identify incomplete studies and technical errors before they are interpreted.
Clinical Evidence for AI Medical Imaging
- Clinical validation is Needed. Several AI imaging products are tested extensively in retrospective and prospective studies.
- Peer-reviewed studies indicate that, for some diseases, AI used in addition to radiologists increases sensitivity and specificity. Combined performance is guaranteed to be superior to individual performances.
- The FDA and CE mark regulatory approvals require the submission of proof of safety and efficacy. These approvals signify clinical, not experimental, application.
- Continuous post-market surveillance assesses real-life performance and limitations. AI Is Decision Support, Not Replacement
The fundamental tenet of AI in medical imaging is augmentation, not replacement. AI doesn’t make the final clinical decisions.
Radiologists review AI outputs within a clinical context. They have patient history, symptoms, and other test results. This human oversight prevents blind faith in algorithms and ensures accountability. AI is a tool, not an expert. This shared model is consistent with professional ethics and preserves patient trust.
Bias and Data Quality Issues
The AI systems are trained with historical data. If the data used to train the model is biased, the model might also be biased.
Bias may also be introduced in the medical imaging process through population or modality-biased sampling. This constraint limits the applicability of the results.
Software vendors are tackling this by making their datasets more diverse and by performing external validation studies. Being transparent about the limitations of a model is paramount for safe use in clinical practice.
Data Privacy and Security Measures
Medical images are associated with sensitive patient information. They also must adhere to AI systems’ data protection requirements. Data security, encryption, and de-identification need to be implemented. Healthcare providers need to be considered.
However, additional protections for cloud-based AI systems against unauthorized access are also necessary. Trust is based on good governance and observance of ethical standards.
AI-Based Imaging Products
AI medical imaging is subject to developing regulations. Authorities now require an unambiguous demonstration of performance, safety, and clinical benefit.
Adaptive algorithms are a new regulatory frontier. Models that evolve over time need to be continuously monitored. These actions safeguard patients and, at the same time, are supportive of responsible innovation.
Explainability in AI Medical Imaging
- Health care providers need to know the reasons an AI system makes a particular recommendation. Explainability adds to the trust in and adoption of the system.
- Visualization tools reveal which regions of an image are contributing to the predictions of an AI. These maps allow radiologists to confirm detections.
- Explainable AI contributes to education and quality control.
- It’s difficult to apply AI in the clinic, because you have no explainability for it.
AI and Multimodal Imaging Analysis
Contemporary diagnosis frequently uses several imaging techniques. AI processes data from CT, MRI, and PET scans. Multimodal analysis enhances the accuracy of diagnosis by integrating complementary information.
AI also connects imaging findings to pathology, genomics , and clinical. This fusion enables precision medicine and individualized therapy planning.
Effect on Patient Outcomes
The primary objective for AI in medical imaging is better patient care. Earlier diagnosis means earlier treatment. Greater accuracy leads to unnecessary procedures.
AI enables standardized care within organizations and at different centers, reducing disparities. In addition, AI contributes to a more efficient healthcare systems.
Barriers to Training and Adoption
Training to use AI is a part of effective adoption. Radiologists must be able to trust and understand the systems. There is need for constant learning.
Economic Effects of AI in Imaging
The AI in medical imaging can lead to cost savings by increasing speed and quality, and decreasing the number of repeated scans. As a result, early detection of diseases will save on the related costs of treatment. But costs for initial investment and integration must be factored in.
AI in International and Remote Medicine
In countries with few trained radiologists, AI is enhancing diagnostic accessibility. Cloud-based imaging AI facilitates remote reading and screening programs. This functionality enhances rural healthcare and global health initiatives.
AI doesn’t replace specialists; it extends their reach.
Prospects of AI in Medical Imaging
- AI will also proceed towards online, adaptive systems.
- Integration with clinical decision support will intensify.
- Regulation, ethics , and explainability will influence the development priorities.
- Emphasis will still be on performing safe evidence-based improvements in patient care.
What is coming Next?
AI in Medical Imaging Research
Research is what pushes AI in medical imaging forward. Testing in academic centers and teaching hospitals largely occurs for new algorithms. These settings enable comparison of AI performance to expert radiologists on validated datasets. So, it is vital that changes are measured and not just assumed.
Clinical trials are incorporating AI applications in imaging workflows. Researchers evaluate the impact of AI on diagnostic performance, reading time, and medical results. Information from these investigations guides regulation and clinical use.
AI medical imaging tools cannot be trusted long-term without robust research underpinning them. Open data also enables faster innovation.
AI and Rare Disease Detection
AI-based medical imaging platforms can detect unusual patterns that even doctors may not see. Using aggregated global datasets to train, AI can pick up on subtle imaging signs associated with rare diseases.
Radiographers receive AI alerts on possible alternative diagnoses. These pushes are for further work and not for final answers. This adjunctive function enhances diagnostic confidence without overriding the clinician Judgment.
Quality Assurance and Error Reduction
Medical imaging diagnostic errors may be caused by fatigue, time constraints or subtle abnormalities. Quality assurance in radiology is influenced by availability of AI as a standardized experience second reader.
AI systems mark inconsistencies, unnoticed findings, or suspicious trends. Radiologists may also examine these warnings prior to completing reports.
Support tools for quality assurance, high quality, and facilitate peer review and education. The institution employs this AI feedback to detect trends in misinterpretations. In the long run, this translates into safer and more dependable diagnostic services.
AI for Pediatric Medical Imaging
Pediatric imaging protocols are optimized using AI. In X-ray and CT scans, AI enables dose reduction without compromising diagnostic quality. This is important because the long-term risk can be reduced.
Pediatric-trained AI models enable accurate interpretations for patients of all ages. This expertise increased confidence for diagnoses that involved growth-related changes. Moreover, pediatric radiologists have access to solutions designed for their specific clinical needs.
The Ethical Responsibility in AI Imaging
Ethical issues influence the development and use of AI in medical imaging. Transparency, accountability, and patient safety remain pressing issues. Physicians need to recognize the boundaries of the system and not place blind trust in what the algorithms report.
Clear documentation and performance metrics enable responsible use. Patients are entitled to that, too. When AI assists with diagnosis, institutions can be transparent about that role.
Ethical AI plays a key role in building trust by ensuring technology works with professional standards and patient expectations.
Continuously Learning and Updating Models
The world of medicine keeps changing, and so should the AI systems. Continuous learning enables imaging AI to improve. Model updates must be validated to verify that performance does not degrade. Healthcare Providers need to monitor version changes and re-assess outcomes.
And regulators are increasingly demanding post-deployment monitoring. This supervision ensures that AI is safe and effective throughout its existence. An update responsibly manages to strike the right balance of keeping innovation fresh and stable in a clinical setting.
Integration with HIS
AI medical imaging solutions should be fully compatible with established systems. PACS and EHR are vital to the imaging workflow. The standards ensure AI solutions are enabled to work across different vendors and organizations. Seamless integration enables adoption and impact in the real world.
Training the Next Generation of Radiologists
People are taught to question AI outputs rather than accept them uncritically. This expertise allows you to maximize your commitment to diagnosis. Exposure during training enhances acceptance of new technology and minimizes barriers to adoption in professional life.
Future radiologists will routinely use AI as a requirement in imaging care.
Defining Success Beyond Accuracy
- Measuring success by accuracy alone is insufficient for AI in medical imaging. Clinical value goes beyond efficiency and usability, and also includes patient outcomes.
- Hospitals are checking if AI can speed up image reporting, make work smoother, and help with quicker treatment.
- User experience matters. Any products that interfere with workflow will have difficulty gaining traction, no matter how accurate they are.
Conclusion
The evidence, regulation, and clinical experience continue to advance. The best systems are those that support clinicians without displacing human effort. No doubt, Artificial intelligence increases speed and consistency.
AI in medical imaging is no longer investigative. It is a rational solution with quantifiable clinical benefits as long as it is used correctly. Very importantly, AI enhances, rather than replaces, clinical findings.

AI in Health care
Digital X-ray vs. Film X-ray: Which is better?

In the last few years, there have been exciting developments in medical imaging. Film X-ray was the traditional way, but recently, some health facilities are using digital X-ray for their radiography. Digital X-ray vs film X-ray: Which one do you consider the best?
This question is quite technical, so I don’t expect a straight answer. Many industries are embracing technology to boost efficiency the health sector included. But how do these two imaging technologies work? Film X-rays produce consistent, reliable diagnostic images; on the other hand, the digital X-ray system has higher speed, quality images, and easy storage and management.
But it turns out technology has made medical imaging work differently. Instead of exposing film, a digital X-ray system uses a sensor to capture the radiation, which is then converted directly into electronic images. The device transmits the information to a computer, and the result is displayed on the screen a few seconds later.
But is digital always the better choice? And what is it exactly that differentiates it from the traditioner imaging system?
What is a digital X-ray?
Digital X-ray is a form of imaging where radiographic images are captured electronically rather than relying on traditional black and white photographic film.
As an alternative to exposing X-ray film, a sensor or digital detector is used to capture the radiation signals. The signals are then converted by the detector into digital data. A computer processes the data, and the images are available on a screen in a matter of seconds. It omits some steps that are traditionally found in radiography.
In film imaging, the technicians have to develop the film to see the outcome. Digital imaging excludes that step. A typical digital X-ray system includes the following:
- An X-ray machine
- A digital sensor or detector
- Computer software for image processing
- A workstation for viewing and storing images
When an image is taken, it displays on the computer monitor immediately. With this, radiographers can adjust the brightness, enlarge the details, and then send the files. This easy workflow is one of the reasons healthcare providers prefer digital radiography.
How Traditional Film X-Ray Works
Film radiography is the orthodox method radiologists used before the introduction of digital x-ray. Although some clinics still use them . In this system, the machine sends X-ray radiation through the body. The radiation reaches a sheet of film placed behind the patient.
Different tissues absorb radiation at different levels. Bones absorb more radiation, while soft tissues allow more rays to pass through. These variations create patterns on the exposed film.
The exposed X-ray film must go through chemical development in a darkroom. The process involves developer chemicals, fixer solutions, and washing stages.
After processing, the film dries, and then it shows the final image. To be honest, this workflow takes several minutes. In busy clinics, it can slow down patient flow.
Still, film radiography has one key advantage. It produces extremely high-resolution images when handled correctly. That dependability is why some institutions continue to use film systems.
The Difference Between Digital X-Ray vs Film X-Ray
The only thing that separates digital and film imaging is the way images are captured, processed, and stored. Let’s make this simple.
Image capture technology
Film X-ray uses photographic film to capture an image of radiation exposure.
Digital radiography, however, captures the radiation signal with an electronic sensor or detector. This is the basic level-out distinction between the two systems.
Image Processing
Film images must be developed with a chemical before the images can be captured. But, a digital X-ray system processes images immediately with a computer software. It only takes a few seconds for a technician to look at the images. There is no wait period.
Storage and Access
The storage is another salient point. Film images are stored or accessed manually from their storage rooms. Digital images are stored in hospital databases or on cloud storage. It makes retrieval much faster and easier.
Image Sharing
Film images must be physically transported or scanned. Digital images can be shared instantly with other specialists through electronic systems.
Workflow Efficiency
Film imaging involves multiple manual steps.
Digital imagine has a straightforward workflow.
This difference improves productivity in high-volume clinics.
Digital X-Ray Machine vs. Film X-Ray Machine
Both technologies focus on similar core equipment. The machine that produces X-rays are somehow identical. However, the imaging components are not the same.
Film X-Ray Machine Setup
A traditional film system typically includes:
- X-ray generator
- Film cassette
- Intensifying screen
- Film processing equipment
- Chemical developer and fixer solutions
Technicians must handle film carefully to avoid exposure errors.
Digital X-Ray Machine Setup
A digital X-ray system replaces film cassettes with detectors.
These detectors may include:
- Flat panel detectors
- CCD sensors
- CMOS sensors
- The sensor captures radiation data and sends it directly to a computer.
- The system then converts the data into diagnostic images almost instantly.
- This simplified process is one reason digital radiography continues to expand worldwide.
X-Ray Film Digitizers: How Conversion Works
Several facilities want to upgrade but already have large archives of film images. This raises an important question: can X-ray film be digitized for modern systems?
The answer is yes.
Clinics usually convert old film records into digital files through scanning technology. Specialized scanners capture the film image and convert it into digital data. Once scanned, the images can be stored in electronic databases.
This process allows facilities to keep historical records without maintaining large film storage rooms.
Digitizing film archives also help physicians have access to files especially if there is need to compare recent and old image.
Advantages of Digital X-Ray
There are so many benefits of digital radiography. They include the following:
Faster Image Results
Digital systems display images within seconds. Technicians can confirm image quality immediately and repeat scans if necessary.
This reduces patient waiting time.
Lower Radiation Exposure
Many digital systems require less radiation than traditional film imaging. Advanced sensors capture more data from smaller radiation doses.
This improves patient safety.
Better Image Enhancement
Digital software allows physicians to adjust contrast, zoom, and brightness.
It reveal details that may be harder to see on film.
Efficient Storage
- Digital images do not require physical storage space.
- Clinics can store thousands of images electronically.
- This reduces operational costs in the future.
Easy Image Sharing
Doctors can send images instantly to specialists across different locations. In addition, it improves collaboration and speeds up diagnosis.
Environmental Friendly
Digital imaging removes the need of chemical processing. By so doing, it removes hazardous chemicals from the workflow.
Facilities also no longer need to dispose of X-ray film and chemical waste.
Limitations of Digital X-Ray
Despite its benefits, digital radiography also comes with some challenges such as:
High Initial Cost
- Installing a digital X-ray system can be expensive.
- The detectors, software, and infrastructure require a larger upfront investment.
- Smaller clinics may struggle with these costs.
Fragile Sensor
- Digital detectors are sensitive equipment.
- A damaged sensor can be costly to replace.
- Proper handling and maintenance are essential.
Dependence on Technology
- Digital systems depend on software to operate efficiently
- Technical failures or network problems can affect system workflow.
- Facilities must maintain reliable IT support.
Advantages of Film X-Ray
While digital imaging dominates modern radiology, film systems have their advantages like:
Lower Initial Cost
- Film systems are cheaper to buy
- This makes them accessible for smaller clinics
High Image Resolution
- Traditional X-ray film can capture images properly
- Many radiologists still appreciate the clarity of film images.
Durability
Digital systems often require upgrades.
Limitations of Film X-Ray
Film imaging also has several drawbacks that modern clinics must consider.
Slower Workflow
- Film requires chemical processing before viewing images.
Storage Challenges
- Film images require physical storage space.
- Not suitable for small clinics because of lack of space.
Chemical Waste
- Film development produces chemical waste.
- Facilities must follow strict environmental guidelines when they dispose of X-ray film and processing chemicals.
- It may attract additional operational cost.
Digital vs. Film in Dental Imaging
Traditional dental X-ray film was the standard for intraoral radiography.
But in modern dental radiography, digital sensors have become the norm. There are a few reasons that dentists choose digital imaging.
The sensor is small enough to be inserted into a patient’s mouth.
Images are displayed immediately on the monitor. Dentists can zoom in on the images and show to their patients.
It boost doctor-patient relationship.
Motion Sensitivity and Image Quality
Patient motion can affect both digital and film imaging.
If the patient moves during exposure, the image may appear blurred.
However, digital systems can sometimes compensate for minor motion artifacts using processing software.
Film images do not offer this flexibility.
If motion affects the image, the radiographer must repeat the scan. It increases radiation exposure and slows the workflow process.
Maintenance and Operational Costs
The cost is what we should also consider.
Film imaging requires continuous supplies.
Clinics must buy:
- X-ray film sheets
- Developer chemicals
- Fixer chemicals
- Cleaning supplies
Digital systems require fewer consumables but depend on upgrade and constant maintenance of the equipment’s.
Facilities must maintain detectors, computers, and imaging software.
Environmental Effect
Film radiography involves chemicals and it should be disposed of properly.
Facilities discard X-ray film at their own risk; they must comply with environmental safety laws.
Silver in film can also contaminate water if not treated properly.
These chemical processes are completely done away with in digital radiography.
This is easier on the environment and on your waste disposal system.
Can Film X-Ray Still Be Useful?
With all the advances in digital imaging, film technology still has its place in certain environments.
Some rural clinics continue to use film systems because they don’t have the infrastructure.
Digital systems need stable electricity and dependable computer networks.
Film imaging can still function with minimal technical assistance..
In these cases, film radiography is still a viable option.
Which One Is Better?
Now the big question is, digital x-ray or film x-ray, which is better?
Digital radiography is rated higher than film x-ray.
It enhances speed, efficiency, and data management. Physicians can get access to images quickly and share them instantly with other specialists.
There is also less radiation exposure for patients.
Film systems may continue to be viable in under-resourced institutions.
But for long-term prospects, digital imaging still is the future of radiology.
The Future of X-Ray Imaging
How has AI transformed radiology today? Cloud storage enables hospitals to exchange imaging information with other healthcare networks.
Digital portable machine units help image in emergency departments, operating theaters, and the field.
These advancements are directly built upon the digital radiography platform.
Film technology has its place in the history of medical imaging. But with the digital transformation, everything about the way healthcare providers diagnose disease is being transformed.
Read also: MRI Machine vs. CT Scan: Which Imaging System Should Your Facility Invest In?
Final Thoughts
The discussion surrounding digital X-rays vs film X-rays is reflective of the larger changes to the medical industry.
Film radiography made a difference in patients’ lives for decades. It gave good pictures, and it helped to diagnose several sicknesses.
But digital imaging brings exciting new opportunities and possibilities.
A modern digital X-ray system produces images at a higher speed, stores them effectively, and facilitates clinical workflow. Doctors can review results faster.
Having said that, each system depends on the cost and storage capacity of the health facility.
So when somebody asks, Which one is better?
For modern facilities, the answer is digital radiography. It increases efficiency, patient safety, and long-term management of images.
AI in Health care
Remote Patient Monitoring in Modern Healthcare

Remote Patient Monitoring (RPM) is not new. RPM is already redefining care delivery. Through digital technology, hospitals and clinics can now monitor patients remotely. The patient doesn’t need to visit the hospital or clinic.
Ongoing care is vital to a patient’s recovery. The good thing about this is that a sick person can still get the desired healthcare right in their home.
With technology advancing by the day, many sectors, the heath included, are enjoying the benefits. Instead of a regular doctor’s visit to the hospital, you can get that done in minutes through special health devices.
The idea is to detect health changes early. The truth is, it is easier to treat an ailment at its early stage. That’s why RPM is now a standard of care, and it helps patients keep track of their health status without visiting the hospital.
What Is Remote Patient Monitoring?
Remote patient monitoring (RPM) is the use of digital technology to collect basic health information from individuals in one location, and then transmit it online to a provider for assessment.
When the data gets to a clinician, he or she will review it. RPM can monitor heart rate, blood pressure, symptoms, and daily routines. Also, they notify you if there are changes in your body system.
Take note of this: RPM is not a substitute for regular doctor visits. However, it complements in-person visits. The main purpose is to augment the physician with real-time health data and facilitate better care decisions, and nothing more.
Best example of Remote Patient Monitoring

One of the best examples of RPM is the ability to monitor hypertension at home. Patients use a digital Cuff to check the readings automatically, then send them to a secure monitoring site.
Clinicians analyze trends, not single readings. This method is more accurate. Whether you check it at home or in the clinic, the result is the same. Moreover, the device allows you to detect trends, such as morning spikes or a reminder.
Most importantly, it means fewer trips to the hospital. Providers can remotely adjust treatment plans. Patients get all the support they need, too. This is the delicate balance that makes RPM successful.
An Example of an RPM Device
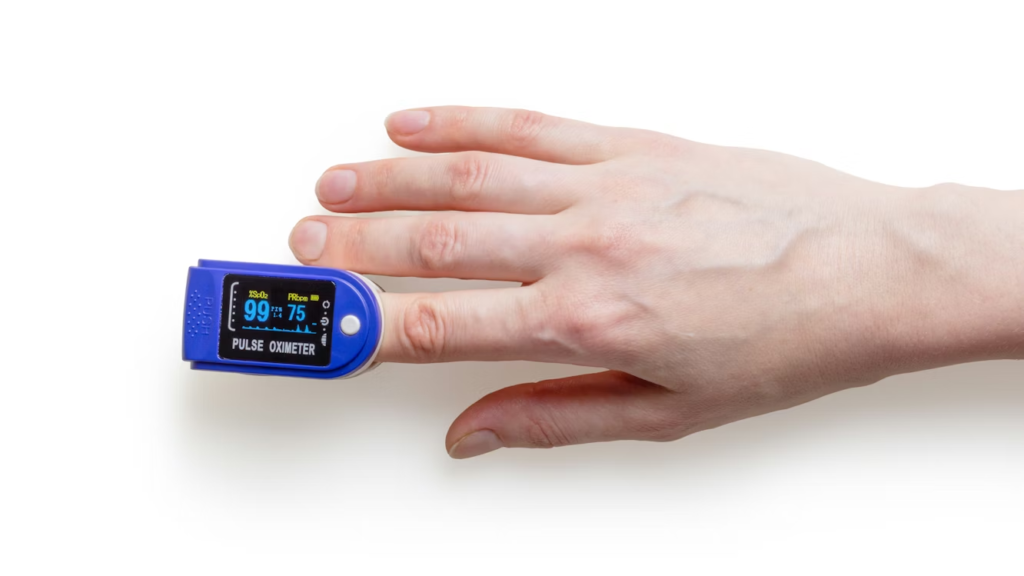
A popular remote patient monitoring (RPM) device is a wearable pulse oximeter. It tests the amount of oxygen in the blood and pulse rate.
A patient wears the device on a finger or wrist. It gathers health data and transmits it through a mobile app or a home hub. The person wearing the device gets an alert if the numbers or codes are outside a safe range.
Pulse oximeters have become common in respiratory therapy programs. Individuals with lung issues, heart diseases, or post-surgery can use it without any complications.
The most appealing aspect of this device is that it is easy to use. Patients do not need skills. All they need to do is wear it on a regular schedule. It vibrates and notifies you of any possible danger.
Who needs remote patient monitoring?
Any person sick can use it. There is no age barrier. However, it is better for people with chronic conditions. Basically, people with long-term chronic health conditions such as diabetes, high blood pressure, asthma, and heart disease benefit more.
In addition, any disease that requires frequent check-ups and periodic adjustments in treatment needs it.
Post-surgical patients can also be eligible. Patients discharged from the hospital recently can be monitored with high intensity at home.
Even in some cases, end-user policies are applicable. As an example, the users of Medicare can be eligible if they have one long-term illness that needs constant monitoring.
Finally, it is the healthcare teams who decide who is eligible. They take into consideration the health status.
How Remote Patient Monitoring Works
First, patients need the health device. Your doctor may recommend that based on your health needs. After that, they will guide the patient on how to use it. The device collects the data, which you send to the dedicated channel for proper analysis.
Every day, or immediately, health workers review the information. Alerts notify you if something is abnormal. There is no delay.
Uses in Healthcare
Remote patient monitoring is used in a variety of medical areas. It helps medical providers track the progress of a condition and the effectiveness of the current treatments. Also, it monitors post-operative recovery by tracking motions, pain, and vital signs of the body.
Mental health services also use remote patient monitoring. They keep an eye on sleep, activity, and daily habits. Individual care plans are developed from the information.
Benefits for Patients
Remote patient monitoring is helpful in diverse ways. Some of the benefits are:
1. Reduces Hospital Visits
It reduces frequent visits to the hospital. With RPM, you will reduce your visits to the hospital drastically. That saves a lot of time, money, and energy.
2. Reduce Stress
Not everyone has a caregiver or someone to look after them. If you are in this category, perhaps you should discuss this with your health care provider. RPM gives you the assistance you may need from caregivers.
3. Can Spot Early Abnormalities
The ability to discover minor alterations in health at an early stage is one of the benefits of the remote patient monitoring devices. The discovery helps to cure the disease before they deteriorate.
4. Comfort at Home
Patients stand in the place where they are used to. They sleep in their own bed. They appear to be less serious and to be happier.
5. More Awareness
Patients can get their health statistics. They know that things are good and bad for the body. It makes them wiser regarding their care.
Benefits for Providers
Healthcare providers derive several benefits from remote patient monitoring. Instead of a single checkup, they can track health numbers on a daily basis. It allows them to know patients better.
Alerts help them know who needs help. These pop-ups inform health practitioners of people that needs assistance the most. It makes work easier, and it saves time.
Remote patient monitoring is a way to keep people out of the hospital. Even at home, doctors and nurses can monitor patients from afar.
Benefits for Healthcare Systems
At the level of the healthcare system, such monitoring makes care work better and makes care work last.
The possibility of patients coming back after a check-up in the hospital is near-zero. The same way, the number of people in the emergency room is reducing by the day. Detecting health problems early can prevent serious conditions from developing.
With more people around the world needing medical care, this system ensures high-quality care without building more hospitals.
Remote Patient Monitoring Programs
Cardiologists also use RPM to monitor patients with heart disease remotely.
- For continuous glucose monitoring. These are medical devices that provide instant glucose information and trends.
- RPM is effective in pulmonary care programs like COPD and asthma.
These examples show that RPM is useful in clinical workflows but not as an independent service.
Remote Healthcare Monitoring in COVID-19.
The coronavirus crisis changed the healthcare provision process. During a large part of the pandemic, government-run hospitals in India were overwhelmed. Then, Remote health monitoring became a veritable approach.
Individuals with mild symptoms didn’t bother to see a doctor because they were closely monitored. Strategically, doctors only attended to patients with serious medical conditions.
Pulse oximeters were useful instruments at this time; they are still of great value. Their work is to check oxygen levels every day and share reports.
This method reduced the high chances of transmitting the disease. It was also easier to know when someone’s health was deteriorating.
Home monitoring is not merely a luxury during the pandemic. It clearly shows the importance during emergencies like the COVID 19.
Lessons
The delivery systems were more effective because of the smooth-flow of information from patient to doctor. The point that patients can manage or monitor their health situation boost their confidence.
Moreover, it is easy to use. You don’t have to be a techie to use it. However, you need proper guidance.
Concrete guidelines do come in handy. Patients were educated on what to observe and when to call to seek help. There were also improvements in the healthcare sector globally.
Data Security and Trust in RPM
Health monitoring technologies require you to have a high level of trust.
Health information is personal. RPM doesn’t expose a patient’s data. There are strong regulations that protect patient data, which is highly confidential.
Information can be encrypted, and layers of protection can be added around information, limiting access. Explicit protocols contribute to ensuring that information is managed appropriately.
Patients are more at ease when they understand how their health information is protected.
Proper supervision and safety protocols ensure that these programs are effective and safe for all.
Clinical Accuracy and Reliability
Monitoring devices for health must comply with stringent safety regulations before they can be adopted. These regulations ensure that the devices provide accurate and safe outputs.
The devices are thoroughly tested and certified by the health authorities. This examination ensures that the data they gather is reliable.
Good systems don’t generate false alarms. False warnings can induce panic and confusion. Good quality devices prioritize distilling complex health data into simple and actionable information.
Doctors are still important. Technology guides them toward better decisions, but it doesn’t replace their education or experience.
The Human Side of Remote Monitoring
Even though remote patient monitoring relies on technology, it needs human effort for proper interpretation.
Patients want reassurance that someone is paying attention to their health condition. Programs perform better when they assist rather than monitor patients.
Routine updates and clear communication ensure that patients get adequate care.
The nurses are still very important. Their warmth, lucid explanations, and prompt attentiveness matter. The best use of technology is when it complements human care and enhances the connection between patients and the healthcare team.
Challenges
Remote patient monitoring has many benefits, but it also has challenges.
Not everyone has the necessary technology. A few patients still do not have a reliable internet connection or a smartphone, which makes using monitoring devices more difficult.
There can be a downside to having too much health data, too. Care teams can get overwhelmed by the information if it isn’t properly filtered.
Patient engagement can vary from patient to patient. Some people are not diligent about using their devices, or they may not appreciate the importance of doing so. Educating the patients and motivating them to do so is necessary.
Remote patient monitoring programs must address these issues. Like software, they must be updated and upgraded.
The Future of Remote Patient Monitoring
The future of RPM will give care teams a clearer understanding of health information and enable each person to receive better support.
AI will be used to sift through and make sense of massive amounts of health data. It also identifies health risks at an early stage, in some cases before a person even becomes ill.
Wearable gadgets, too, will get better. They are light and comfortable to wear on a daily basis. Multiple sensors could be integrated into clothes or watches so they can be used without interrupting day-to-day life.
Healthcare systems will also integrate better. Various devices and applications will have the means to exchange data seamlessly, enabling better integration among them. Care teams can now access a more complete picture of a person’s health.
But remote patient monitoring in the future won’t stop at passively monitoring your vital symptoms. It will anticipate complications at an early stage and aid in treating patients before the diseases lead to serious conditions.
Why It Is Here to Stay
RPM solves critical healthcare challenges. It brings care closer to the patient and reduces cost. It’s also enabling people to achieve better health outcomes.
This mode of care is useful for seniors and chronic-illness patients. These populations usually need constant check, and remote monitoring enables them to do that without making hospital visits too often.
A lot of patients now expect healthcare stress-free and connected. Remote patient monitoring meets this demand by enabling care delivered at home, with digital tools.
And because it increases access, decreases cost, and promotes better health, RPM will also be a big part of the future of health care.
Read also: AI in Medical Imaging: What is Coming Next
Final Thoughts
Health care is evolving, and care is migrating closer to where people live. A trusted technology can improve care.
When embraced with care and consideration, Remote Patient Monitoring can make patients feel better, and healthcare systems as well play a more significant role in the future of healthcare.
-

 Uncategorized4 months ago
Uncategorized4 months ago6 Best Heatmap Plugins – I Test, Review and Compare
-

 AI in Health care3 months ago
AI in Health care3 months agoRemote Patient Monitoring in Modern Healthcare
-

 Diagnostic & Hospital Equipments4 months ago
Diagnostic & Hospital Equipments4 months agoWhat Are Medical Devices? Types and Uses
-

 AI in Health care1 month ago
AI in Health care1 month agoDigital X-ray vs. Film X-ray: Which is better?
-
 Review and guides3 months ago
Review and guides3 months agoCPAP Machines Buying Guide: The Best Models Doctors Don’t Recommend
-

 Home and selfcare3 months ago
Home and selfcare3 months agoBest Pulse Oximeters for Home Use
-
 Diagnostic & Hospital Equipments1 month ago
Diagnostic & Hospital Equipments1 month agoDEXA Bone Density Scanning: What You Need to Know About Bone Health
-
 Diagnostic & Hospital Equipments4 weeks ago
Diagnostic & Hospital Equipments4 weeks agoPET Scan Machines: Understanding the Technology, and Usage