Home and selfcare
Most Accurate Home A1C Test Kits (compared to lab results)
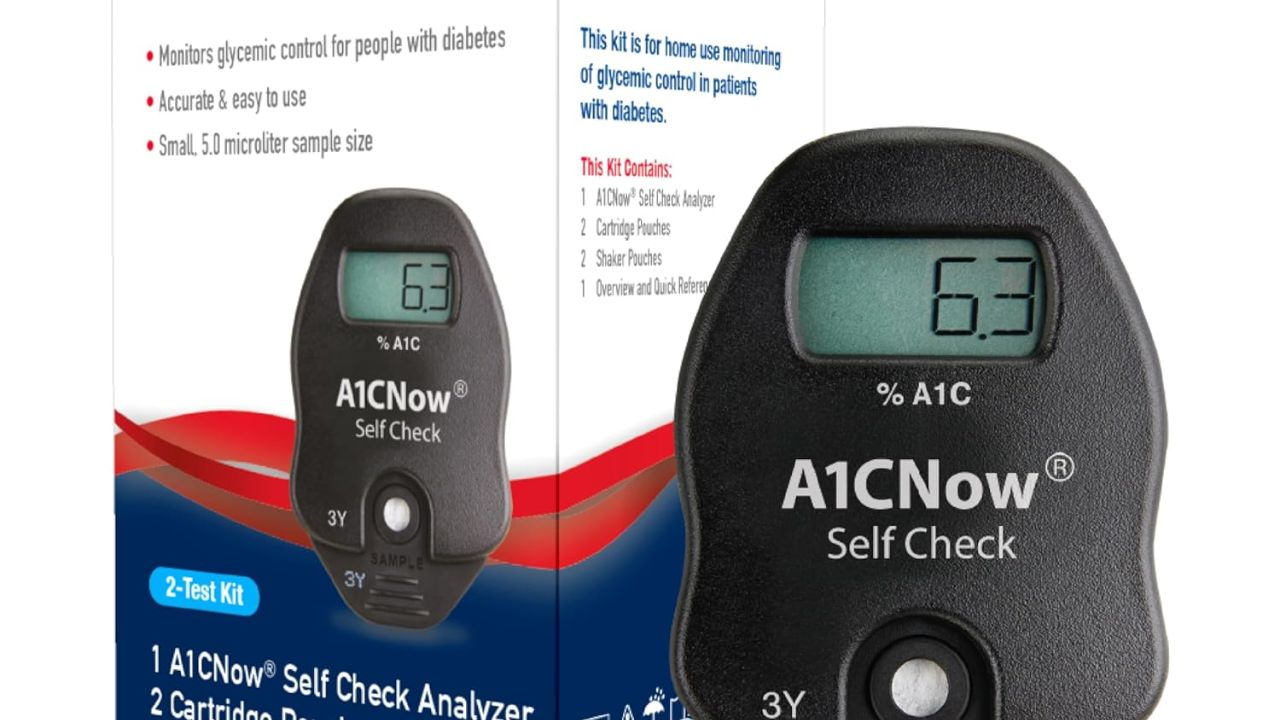
Do you think home A1C tests kits can provide the same results as a lab test? Many people are skeptical of using it and would want to know how accurate they are. Some use this test kit to manage diabetes, monitor prediabetes, or track long-term blood glucose levels.
Home A1C test kit manufacturers have been contending for years that their products provide results that are as good as laboratory results. Some A1C test kits are good; however, not all are accurate. They only help spot trends and are not for clinical evaluation.
This article will highlight the best A1C test kits for self-check and who needs them.
What Is an A1C Home Test?
An A1C home test estimates your typical blood glucose levels for the previous two to three months. Unlike the results of daily finger-stick glucose tests, it doesn’t reflect real-time changes. It is a measure of blood sugar control over time rather than at a single point in time.
Home A1C test kits require only a small drop of blood, which is usually collected through a finger prick. That sample is either:
- Sent to a lab for processing
- Tested right at home with a handheld device. It is expressed as a percentage.
- Higher percentages mean higher average blood sugar levels.
How an A1C Home Test Kit Works
A1C is a device that measures how much sugar has been attached to your red blood cells over the past 2 to 3 months. Glucose normally attaches to hemoglobin, the protein that red blood cells use to carry oxygen. The greater the level of your average blood sugar, the more glucose attaches to that hemoglobin. This percentage is your A1c result.
Several home A1C tests begin by taking a drop of blood from your finger. You clean your finger, use a tiny lancet to draw a few drops of blood, and adhere to the instructions in the kit meticulously. Following that, “What do you do next?” is determined by “Which version of the test do you have?”
Some at-home A1C kits require that you mail your blood sample to a CLIA-accredited lab. The sample is tested by the lab using standardized methods that are comparable to those that are used in hospitals and clinics. Results are typically available within days and delivered digitally.
Other home A1C tests, such as instant self-read devices, test the blood right away on a small handheld analyzer. These tests yield results in minutes, but they are more sensitive to proper timing, sample size, and storage conditions.
The result in both cases is an average of your blood sugar levels—not the moment-to-moment data you get with the latter method. That’s why an A1C home test is better for long-term tracking instead of immediate glucose changes.
When administered properly, a good home A1C test can provide lab-like results and a reliable window into how well your blood sugar is being managed.
Who Needs an A1C Home Test?
An A1C home test is mostly used by:
- People living with type 1 or type 2 diabetes
- Individuals with prediabetes
- Adults at risk of diabetes due to family history, weight, or lifestyle
- People monitoring treatment effectiveness between clinic visits
- Those who prefer privacy or limited clinic visits.
Also read: Best Health Tech for Managing Multiple Chronic Conditions
How Accurate Are Home A1C Tests Compared to Lab Results?
The best home A1C test kits are developed to be very similar to lab A1C testing and usually have a margin of error of ±0.5% compared to a result from a venous blood draw. Accuracy depends on:
- Method of testing (lab-analyzed vs. instant reader)
- Handling of samples
- Certification of the laboratory
- User technique (taking the test)
Tests from CLIA-certified labs tend to be more concordant with clinical results. Instant tests that are cleared by the FDA can also be trusted, but you have to be very careful with them.
Most Accurate Home A1C Test Kits (Compared to Lab Results)
Best Overall: LetsGetChecked A1C Home Test

What differentiates LetsGetChecked is its mix of accuracy, clinical oversight, and user experience. It is widely considered the most accurate at-home A1C testing kit when compared to lab results.
Features
- Finger-prick sample of blood
- The sample is tested in a CLIA-certified lab.
- Results usually take about 2–5 days.
- When compared to a standard lab, A1c testing accuracy was found to be very similar.
- FDA-approved collection technique
Because the testing is done in a professional lab, there’s less room for error. This is in contrast to how most doctors check A1C in the office.
About LetsGetChecked
- Follow-up from a nurse is optional.
- Clear digital results with explanations from a clinician
- Good for initial testing as well as ongoing monitoring
- Sample must be mailed; no instant results
This test is great for those who want the reassurance of a lab test but don’t want to go to a clinic.
Everlywell HbA1c Home Test

Everlywell’s HbA1c home test has a solid reputation for its low cost and good agreement with lab comparisons. It is widely picked by people who test sporadically rather than every month.
Features:
- Blood sample from a finger stick
- Labs processed through a CLIA-certified lab
- Results are typically back within a few days.
- Consistent with lab-based A1C results
- Precise numerical results along with reference ranges
Everlywell strikes a good balance between value and quality when it comes to testing accuracy.
What You Should Know about Everlywell
- No real-time results
- The collection method is easy.
- Ideal for regular monitoring
- Fewer personalized follow-ups than several high-end services
This product is designed for those users who only want accurate A1C results and do not require any other clinical features.
Best for Follow-Up Care: myLAB Box Hemoglobin A1c Screening Test

myLAB Box prioritizes testing with clinical continuity, so it can be an effective option for follow-up care after you’ve been diagnosed or your treatment has changed.
Features:
- Finger-prick blood sample
- Analysis in the lab
- Accuracy similar to the conventional laboratory test
- Results are verified by a team of healthcare professionals.
The test is NOT a replacement for routine care.
What to Know About myLAB Box
- Physician-reviewed results
- Clear interpretation for treatment tracking
- Great for trend monitoring over time
- You have to mail in your sample.
A1CNow SELFCHECK

A1CNow SELFCHECK stands apart from the other options. There is no need to send specimens to a lab, as you get the results instantly at home.
Features:
- Finger stick blood sample
- Instant digital reading
- FDA-cleared for home use
- Results in minutes
Research suggests that A1CNow SELFCHECK results can be fairly comparable to the lab results, but accuracy is highly dependent on technique and storage conditions.
About A1CNow SELFCHECK:
- No lab processing
- Good for frequent monitoring convenience
- More variability than lab tests
- Use for trend monitoring, not for diagnosis.
This test is for the experienced user who wants speedy feedback between clinical visits.
What to Know Before Choosing a Home A1C Test
- Lab-Based Vs. Rapid Tests
Lab-home A1C tests tend to be more accurate. Speed and convenience come at the expense of accuracy with instant tests.
- Certification and Oversight
Make sure the test has been processed in a CLIA-certified lab or approved by the FDA. That has a direct impact on reliability.
- Sample Handling Matters
Even the most reliable home A1C test has the potential to lead to false conclusions if:
- Sample is insufficient
- Instructions are not followed
- It’s expired or invalidated
Home Testing Has Limits
Home A1C tests are not made for making emergency decisions or for diagnosis without the involvement of a care provider. They are tools for awareness and monitoring.
Understanding Your A1C Result at Home
Usual ranges for HbA1c:
- < 5.7%: Normal
- 5.7% to 6.4%: Prediabetes
- ≥ 6.5%: Diabetes.
Are Home A1C Kits Accurate for Monitoring Long-Term R1?
Yes, if they consistently use the same methods and tests. Many people who take home A1C tests stick with one brand over time to monitor trends rather than a single reading. The usefulness of consistency
The best-performing home A1C test kits compared with the lab are those that:
- Are taken regularly
- Are followed by medical advice
- Are interpreted together with other health information
What Makes an A1C Home Test “Reliable and Accurate?
How accurate your home A1C test is depends on more than just the brand. Here’s what to keep in mind:
Make sure that the test is certified by a CLIA-approved lab. These kits have tight quality controls. Also, your blood sample has to be stable when it’s shipped. And you must understand the how to use the kit. If you don’t collect the sample correctly, that is where it can produce wrong results.
Errors in A1C Results
A1C tests aren’t totally exact, even in hospitals. Most doctors think a 0.5% difference is okay. So, if you get 6.8% at home, the lab might read anywhere from 6.3% to 7.3%.
This doesn’t mean the test is bad. It just means you should look at the overall trend, not just a single result. Consistent results are what really matter.
How Often Should Home A1C Tests Be Used?
Doctors suggest that people with diabetes use the A1C test kit every three months, and twice yearly for stable prediabetes. However, patients are to follow their doctor’s advice.
How to Prepare for a Home A1C Test
Make sure your hands are clean and warm so the blood flows well. And when you’re testing, don’t use kits that are past their expiration date. Test at room temperature. To get the right result, just do what the instructions say.
If You Test at Home, Double-Check A1C Results at a Lab
If you receive an unusual or excessively high reading, use a lab test to confirm it. This is vital because it could cause you to change your medication, food, or treatment plan.
An A1C test you do at home can give you some info about your health, but, you shouldn’t rely on it.
Why Are Some Home A1C Tests More Accurate Than Others?
Accuracy depends on how it’s done, not what they say. Home A1C tests that use labs that have been certified follow the same rules as clinics. That includes making sure everything is set up right, keeping an eye on quality, and reporting results the same way every time.
Home tests that give you instant results cut out shipping time but can change based on the user.
How big the sample is, when you do the test, and how you store it can affect the results. This explains the differences in consistency, which is, as a general rule, why home tests with lab tests are as accurate.
Using Home A1C Results in Conversations with Doctors
Home test results, like the A1C, can help when you talk to your doctor, but only if they’re from trustworthy companies. Doctors usually trust home A1C tests more if they’re done by labs with CLIA certification or devices cleared by the FDA because these follow quality standards.
Bringing your A1C results to appointments helps show patterns over time, instead of just one reading. This is helpful for checking glucose control in the long run, seeing if lifestyle changes are working, or how well you’re sticking to a treatment plan between visits.
For the most reliable result, make sure it’s consistent and well-documented. Write down the test brand and date, and whether the sample was processed in a lab. This helps your doctor understand the data. Home A1C results that are close to the clinic numbers can help with Home A1C tests are helpful, but don’t skip your regular doctor visits.
Tell your doctor which home test you’re using and how often you test so they can properly understand your results. It’s best to use home tests alongside your doctor’s tests to help make better healthcare decisions together, instead of making choices based on your home test alone.
Frequently Asked Questions
1. Can doctors trust home A1C test results?
Yes, especially when the test uses a certified laboratory or an FDA-cleared device.
2. Should home A1C results replace lab testing?
No. Home tests support monitoring but do not replace clinical lab tests.
3. How should I share my home A1C results with my doctor?
Bring a record showing the test brand, dates, and results.
4. What if my home A1C result differs from my lab result?
Small differences are normal, but confirm large gaps with a lab test.
Read also: Portable vs. Tabletop Nebulizers: Which is Better for Home Use
Final Thoughts
Home A1C testing has added to diabetes care. For accuracy, use any of the above home A1C test kits. However, the best for you will depend on what you’re looking for, such as speed, cost, follow-up care, or how clinical it is. If accuracy is what you’re after, lab-processed home A1C tests are a great option.
Note: An AIC home test kit cannot replace routine medical checkups in the hospital. It is a self-device that helps monitor your blood sugar level.
Hope this is helpful. Drop your comments below. Also like and share on your social media pages.
Home and selfcare
DIY Health Monitoring: What’s Worth It and What Could Cost You

With some simple home medical tools, you can monitor your health. The truth is that you don’t wait for something to go wrong before you check your health, and the interesting part is that you can do it yourself. DIY health monitoring is necessary; however, you must understand the process and know the medical device to use.
DIY health tracking is open to everyone, especially now that health costs are soaring, but it shouldn’t substitute for doctor visits. Let’s talk about what really works so that you don’t spend money on worthless gadgets.
Why DIY Health Monitoring is Necessary
Despite the huge amount most countries propose for their health sector, health care is still costly. According to one of the articles in National Institutes of Health, global life expectancy rose from 46.5 in 1950 to over 73 in 2025. This resulted in seniors needing more long-term health care.
And in certain cases, there are no symptoms until it gets to the last stages. To curb this menace, we now have home kit tools. DIY health monitoring gives instant feedback.
Heart rate, sugar level, and many more can be monitored with a DIY tool. It shows you vital information about your health. It sounds good, right? But if you don’t get it right, it can worsen the situation.
Use of DIY Health Monitoring Devices
Some devices support your health if you use them correctly. They present your health trends, but they cannot diagnose a disease. Fitness trackers, for instance, motivate you to exercise, and display activity records. Blood pressure monitors detect early hypertension warning signs, while Glucose monitors guide people with diabetes. These devices address potential issues so that the user can act fast.
For Tracking Heart Rate
Heart issues are one of the causes of sudden deaths. Although there are signs of heart failure which includes: frequent shortness of breath, constant weakness, and swelling in the legs or stomach. In this situation, anyone diagnosed of heart failure needs portable ECG monitors or smartwatches.
Sleep Tracking
If you notice regular waking or unpredictable patterns, adjust your schedule, go to bed early, and do not take caffeine one hour before you sleep. There are more important things about sleeping well than the number that appears.
When DIY Health Monitoring Saves Money
When you detect an illness early, the chances of curing it are high. Most health issues, like cancer and diabetes, are always detected late, which is why the chances of survival are almost impossible. Early detection can also reduce treatment cost.
Tracking activity also promotes steady movement, which help in reducing the risk of diabetes and cardiovascular disease. You can start by identifying a health challenge you want to monitor. If it is a sleep disorder, use it to improve your sleep or manage blood pressure. If you get an abnormal report, please see your doctor.
The Hidden Risk in DIY Health Monitoring
That you see what is presumed as a good reading on a wearable does not guarantee that there is no hidden health challenge. Cholesterol, inflammation, or disease in its early stages may not show up on consumer devices.
This is to tell you that you shouldn’t depend on your digital tool, as it can produce false readings, which will require the wrong treatment. You can start by identifying a health challenge you want to tackle. If it is a sleep disorder, see how to improve your sleep. Manage blood pressure. Increase activity. If you get an abnormal report, please see your doctor.
How to Approach DIY Health Monitoring
Ask yourself why you want the data. Is it to monitor your health or replace the regular medical checkup? You can use it monitor your health, but you should skip a medical checkup, especially if you have been diagnosed with a chronic illness.
To follow this approach,
- Choose doctor-approved tools. Follow instructions carefully.
- Record results
- Avoid self-diagnosis.
The numbers on the monitor may be incorrect. Always recheck and send the report to a clinician for proper evaluation.
Who can use DIY Health Monitoring Devices?
According to a report, approximately 41 percent of U.S. adults reported using wearable devices for health tracking in 2024, up from about 30 percent in 2020. That means over 108 million people are now tracking steps, heart rate, or other metrics regularly. However, only about 18.5 percent use them daily, and few share data with clinicians.
Despite growing adoption, the usage patterns differ by age, income, and perceived usefulness — suggesting that many people adopt DIY health monitoring casually rather than strategically.
Accuracy in DIY Health Monitoring
Knowing how accurate your wearable is makes all the difference. Modern analyses show that some devices have high sensitivity and specificity of about 95% when detecting conditions like atrial fibrillation, which is a major heart rhythm disorder.
But that high performance doesn’t apply to every metric. How accurate a result is depends on the type of device, sensor quality, and how you wear it.
Step Count and Activity Tracking: Useful but Imperfect
Activity trackers are some of the most common DIY health monitoring tools. Research indicates that people who use wearable devices are twice as likely to meet recommended weekly activity levels compared with non-users.
However, step count accuracy is not perfect, and it differs by device and context. Some models underestimate steps during daily use, especially during erratic movement, which highlights the importance of interpreting these figures as estimates, not precise biomedical measures.
Heart Monitoring Strengths and Weaknesses in DIY Health Monitoring
Monitoring your heart rate and rhythm is one of the most tangible benefits of DIY health monitoring. Devices now detect signs of irregular heart rhythms and arrhythmias, offering early alerts that may prompt medical follow-up. Research shows wearables can reach high levels of detection accuracy for certain conditions like atrial fibrillation.
Still, devices are not clinical ECG machines. They may miss subtle signals or produce false positives under specific conditions, and data interpretation outside the clinical context can mislead users. Use heart metrics for trend awareness, not diagnosis.
Sleep Tracking and Its Limits in DIY Health Monitoring
We need this. DIY sleep tracking is useful because of the effects of poor rest. Consumer devices estimate sleep duration and patterns that can motivate healthier routines. So, their ability to detect true sleep stages like REM or deep sleep is somehow limited compared with polysomnography, the clinical sleep lab standard.
Readings for wake time and total sleep duration sometimes are not the same with lab reports, which means you can only adjust your sleep pattern, but if you have serious sleep concerns, see a doctor or go to the hospital for a proper diagnosis.
Challenges in DIY Health Monitoring
One of the biggest liabilities in DIY health monitoring is inconsistent data. Consumer devices often perform differently in lab conditions compared with real-life use, and environmental factors, skin tone, motion, and placement affect results.
In addition, many metrics are not medically regulated. Only a subset of consumer monitors undergo rigorous evaluation. Users must know that not all data is clinically validated.
DIY Health Monitoring for Chronic Conditions
Some people use DIY tools to manage long-term diseases like diabetes, hypertension, and heart disease. For certain conditions, continuous glucose monitors and blood pressure devices provide invaluable trend data that supports better self-management.
Studies show that data gaps during abnormal glucose periods are common among diabetes patients, which undermines the potential benefits of DIY glucose monitoring if the user does not wear the device consistently.
Tracking health metrics constantly can affect mental well-being. A correct number gives you a sign of relief, while frequent alerts and different figures can make you feel anxious.
How DIY Health Monitoring Integrates With Healthcare Systems
DIY health monitoring is not the final solution. Although, it can support clinical care, especially when remote monitoring and telehealth are involved. Wearable use has been linked with higher telehealth adoption among aging adults as long as socioeconomic barriers like education and income are addressed.
Best Practices for DIY Health Monitoring in Everyday Life
If you don’t know how to use some of these medical home devices, trust me, you will regret buying them. To ensure that a selected device works, do the following:
- Buy the device you need
- Choose a medical-approved device.
- Recheck like every 2 weeks, not daily.
- Cross-check unusual results with clinical assessments.
Research-Backed Devices in DIY Health Monitoring
Here are categories that show stronger reliability in independent research:
Clinically Validated Blood Pressure Monitors
Home blood pressure monitoring has strong backing from organizations like the American Heart Association. Validated upper-arm cuff monitors perform far better than wrist models.
Look for devices listed on validated device registries, such as STRIDE BP, or those cleared by regulatory bodies like the FDA.
Best for:
- Managing Hypertension
- Monitoring medication response
- Early detection of high blood pressure
Avoid:
Cheap, unvalidated wrist monitors.
Read also: Upper Arm vs. Wrist Blood Pressure Monitors: Which Should You Buy?
ECG-Enabled Smartwatches
Some smartwatches now include single-lead ECG functionality. Studies show high sensitivity for detecting atrial fibrillation when compared with clinical ECG devices.
These watches are useful if:
- You have palpitations
- You are at a higher risk of arrhythmias
- Your doctor recommends monitoring
They are not replacements for hospital ECG machines. But they can trigger a timely medical evaluation.
Continuous Glucose Monitors for Diabetics
Continuous glucose monitor have strong clinical benefit for people with diabetes. They reduce hypoglycemia risk and improve glucose control when used appropriately. Use the tool if you have a condition that requires it.
Pulse Oximeters With Medical Clearance
Pulse oximeters became common during respiratory illness outbreaks. Medical-grade devices can reliably detect oxygen saturation trends.
However, accuracy may vary with skin tone and peripheral circulation. They work best for people with respiratory conditions and can only be use under medical advice.
Weight Scales With Body Composition Metrics
Smart scales estimate body fat percentage and muscle mass through bioelectrical impedance. They track trends, not exact numbers. Use them to monitor the direction of change, and not precise body composition.
Devices that are a waste of money in DIY Health Monitoring
Some categories sound advanced but lack strong evidence, examples are:
At-Home Food Sensitivity Kits
Unfortunately, many people depend on IgG antibody testing. Major allergy organizations state that IgG testing does not diagnose food intolerance. Elimination diets should be supervised by professionals.
Broad Hormone Panels Without Clinical Indication
Hormones change during the day and when menstruating. Random testing usually produces misleading results. To prevent this, consult a health practitioner for proper medical evaluation.
Microbiome Subscription Testing
The gut microbiome is complex and still under study. Results may lead to generic supplement suggestions rather than targeted treatment.
How to Evaluate a DIY Health Monitoring Product Before Buying
Before spending money, ask:
- Has this device been validated in peer-reviewed studies?
- Is it cleared or regulated by a recognized authority?
- Does it solve a specific health need I actually have?
- Can a clinician interpret the results if needed?
If you cannot answer yes to most of these questions, maybe, you don’t need the device, it will be a waste of money.
FAQs About DIY Health Monitoring
1. Is DIY health monitoring accurate enough to replace doctor visits?
No. It makes people more conscious about their health, but it does not replace clinical exams, laboratory tests, or professional diagnosis.
2. Can wearable devices detect serious heart problems?
Some devices can detect irregular rhythms like atrial fibrillation with good sensitivity, but confirmation requires medical testing.
3. Is it safe to use a continuous glucose monitor without diabetes?
Most medical guidelines do not recommend CGMs for people without diabetes unless supervised by a clinician.
4. Why do my wearable numbers change daily?
Several factors, like Hydration, stress, poor sleep, and device placement, can affect readings daily. You can check daily, maybe, in the morning, and before going to bed.
Wrapping Up on DIY Health Monitoring
DIY health monitoring should make you understand your body. You can use it to monitor your health; however, your health improves through healthy lifestyle choices, not accurate numbers derived from a tech gadget.
If you must use this approach, don’t depend on the data alone. For a complete diagnosis, you need a lab test. These home medical kits are there to support your health and not take the place of a doctor.
Diagnostic & Hospital Equipments
Blood Pressure Monitor Problems: Common Errors and How to Fix Them
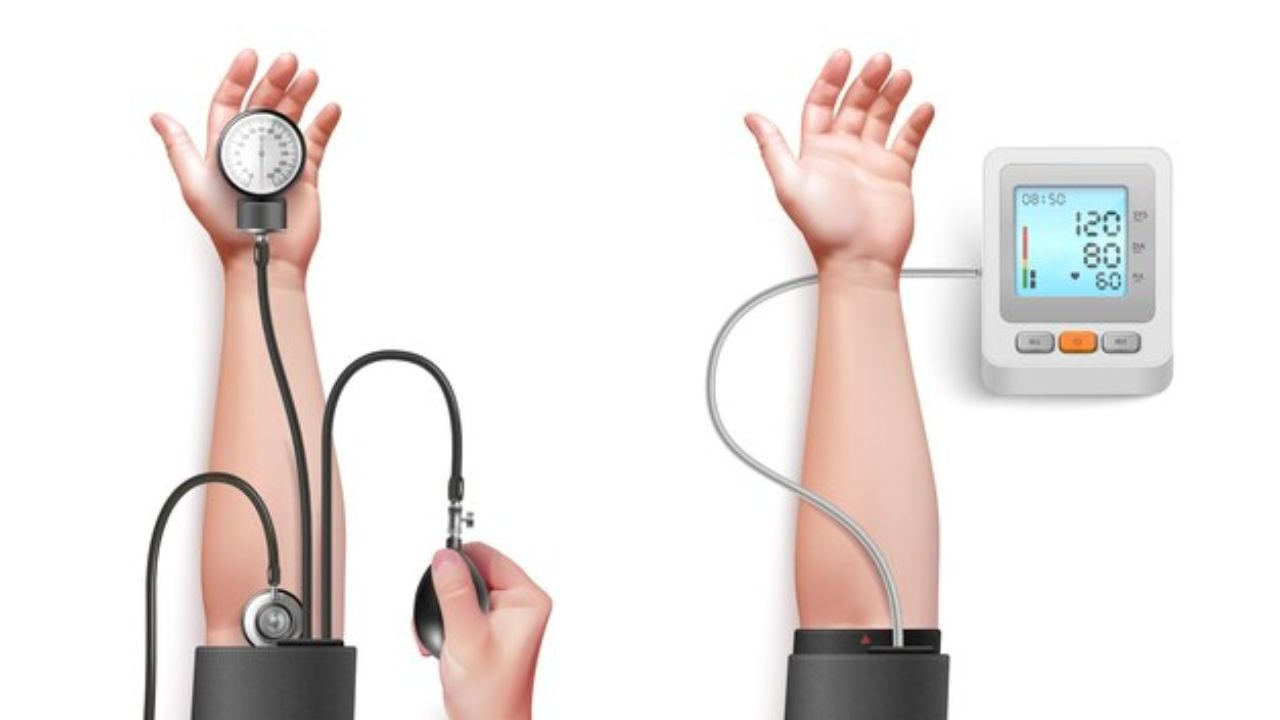
Checking your blood pressure at home is supposed to make you feel relaxed. For so many, it does not happen like this. Sometimes the numbers don’t look the same even after repeating the process. This is when they start to doubt the credibility of the device. What are the common blood pressure monitor problems? The answer and how to fix them are below.
Incorrect readings at times is not about the device but not knowing how to use it. Basically, blood pressure monitors at home are most often trustworthy.
When you get the hang of these things, especially if you’re someone who checks blood pressure often, it helps a lot. Accurate measurements keep everything in balance. So, spotting real changes becomes easier and there’s less worry involved. Knowing common mistakes and fixing them can make you more comfortable with taking blood pressure at home. This approach not only simplifies the task but also enhances its usefulness.
Now, let’s break it down: what exactly is a blood pressure monitor?
A blood pressure monitor is an instrument that measures BP. It determines the force of your blood on your artery walls as your heart beats. You receive two numbers: systolic (top number) and diastolic (bottom number). This pressure becomes different if you are moving, feeling anxious, standing up or down, or if your health conditions change.
These days, people have blood pressure monitors in their homes. Instead of going to clinics to check your vital signs, you can do it at home. However, you must be skillful in this. Using these devices in the correct way produces the actual reading.
How a Blood Pressure Monitor Works
To start, wrap the cuff around the upper arm or wrist. Next, inflate the cuff until blood flow stops. It gently compresses the artery, which reduces or nearly stops blood flow for a short period. Then, slowly deflate it and record measurements as blood begins flowing again. The device picks up signals from the artery and notes pressure changes.
You’ll see two numbers on digital monitors: systolic (when your heart beats) and diastolic (when your heart rests). Some machines are digital; others require manual operation.
Types of Blood Pressure Monitors
Blood pressure monitors come in a variety of forms, but they all operate on the same basic principle. Upper-arm monitors are often recommended because they measure pressure near the heart and usually provide the most reliable readings when used properly. Wrist monitors are more compact and portable, but they require careful positioning at heart level to avoid incorrect results.
Many users struggle with maintaining this position accurately. In clinics, manual devices rely on a stethoscope and a person’s ears for listening. On the other hand, digital home devices simplify the process for everyday use.
Why Proper Use Matters
The right way to use a BP machine is very important. If you don’t use it correctly, the device won’t work well. Stress, moving around too much, sitting poorly, and not putting the cuff on right can mess up the connection between your heart and the machine. This can lead to wrong readings. But if you always use blood pressure monitors correctly, they let you see trends in your health instead of just random numbers.
Read also:Best Blood Pressure Monitors for Seniors: Doctor-recommended
Blood Pressure Monitor Problems That Affect Accuracy
Choosing the Incorrect Cuff Size
Picking the wrong cuff size is a common problem with blood pressure monitors. You’d be surprised how often this happens, especially with shared or used devices. A tight cuff can make your blood pressure seem higher than it is, while a loose one might show a lower reading.
People with larger or smaller arms often end up using standard cuffs that don’t fit well.
Solution:
- Measure the circumference of your upper arm and use the cuff size recommended by the manufacturer.
- If your arm measurement falls between two cuff sizes, choose the larger one.
Incorrect positioning of your arm and body
Your blood pressure can vary based on your posture. If your arm hangs down, crosses in front, or sits too high, the reading may be wrong. Many people check their blood pressure while relaxing on a couch or rushing around standing up, which isn’t ideal.
Solution:
- Sit up straight with your back supported.
- Place both feet flat on the ground and relax.
- Place your feet flat on the ground.
- Rest your arm on a table so the cuff lines up with your heart.
- Let your shoulders drop and keep your hand loose, not tense.
This position ensures a consistent balance between your heart and the cuff, which helps the device accurately measure pressure.
Measuring Immediately After Activity
One mistake people make when measuring their blood pressure is doing so immediately after walking, climbing stairs, exercising, or even running around the house to do something. Blood pressure increases temporarily for all people, even healthy individuals, after physical activity. This makes people believe they have high blood pressure when, in fact, the reading is just responding to movement.
The solution is to:
- Sit for at least 5 minutes and be quiet before taking the reading.
- Don’t do any exercise, or any other physically demanding activities, before checking.
Blood pressure monitors measure systolic and diastolic blood pressure, and that is what you’re ultimately trying to track.
Talking or Moving During Measurement
When using a blood pressure monitor, it’s important not to talk or move because these actions can interfere with the device’s ability to get an accurate reading of arterial pressure. If you chat or shift your arm, the result might be incorrect. Distractions like these happen often but they can cause false readings.
Solution:
- Remain still during measurement
- Don’t talk, laugh, or fidget in your chair
- Position your arm comfortably and relax your palm so that it faces up.
The blood pressure monitor only measures blood flow to the arteries, so it needs you to be still.
Measuring Over Clothing
Never place the cuff over rolled-up sleeves when taking your reading. Doing so will prevent the cuff from fitting properly and could lead to inaccurate results. Pressure can make the cuff warp and strain. Many do this for convenience but overlook the consequences.
Solution:
- Don’t put any kind of fabric over the cuff
- Avoid tight or thick clothes on your upper arm
- For precise measurements, let the cuff touch your skin directly.
Device-Related Blood Pressure Monitor Problems
Low Battery or Power Issues
Digital blood pressure monitors require good battery power to function properly. When batteries are low, the monitor may give no readings, give incorrect readings, or give the user error messages. Most often, the user does not know that the monitor is giving inconsistent readings because of a dead or weak battery.
How to fix it:
- Change batteries regularly. Pay attention to the battery guidelines on your monitor.
- Avoid combining old and new batteries.
Devices perform better with fresh batteries, leading to fewer incorrect readings.
Poor calibration
Blood pressure monitors lack calibration. Over time, sensors inside the monitor may drift as you use it. This drift can lead to significant issues if you rely on these readings for medication or lifestyle adjustments.
How to fix it:
- Get your device checked every one to two years
- Review the results from a clinic visit.
- If an older device can’t have its calibration confirmed, it’s time to replace it.
Using Wrist Monitors Incorrectly

Wrist monitors are handy, though they’re more prone to positioning errors compared to upper-arm devices. Even a tiny misplacement can lead to big differences in the readings. So, here’s what you do:
- Make sure your wrist stays at heart level while measuring.
- Sit quietly and don’t bend your wrist.
- Also, stick closely to the manufacturer’s instructions.
If used correctly, wrist devices can provide accurate results, yet they need more focus on posture.
Timing Errors That Distort Readings
Measuring at Inconsistent Times
Blood pressure naturally changes throughout the day. Morning readings often differ from evening readings due to hormones, stress, and activity levels. Measuring at random times creates confusion and makes it harder to identify trends.
How to fix it:
- Measure at the same time each day.
- Common choices are morning and evening.
- Record readings consistently.
- Consistency supports better long-term balance in monitoring and decision-making.
Measuring Too Frequently
Checking blood pressure multiple times within minutes can cause fluctuating results due to anxiety or squeezing the arm too much. People end up chasing perfect numbers, but that’s unrealistic. For a better approach:
- Take two readings with a one-minute gap and note the average
- Avoid constant checks throughout the day unless instructed by a professional.
Lifestyle Factors That Affect Accuracy

Stress and Emotional State
Emotional stress raises blood pressure temporarily. Measuring during moments of worry, frustration, or panic can result in misleading numbers.
This is a hidden problem many people overlook.
How to fix it:
- Sit quietly and breathe deeply before measuring.
- Avoid checking blood pressure during emotional moments.
- Create a calm routine around measurement.
- Mental calm supports physical accuracy.
- Caffeine, Nicotine, and Alcohol
Stimulants and depressants can alter blood pressure for hours. Coffee, energy drinks, cigarettes, and alcohol all affect readings.
How to fix it:
- Avoid caffeine and nicotine for at least 30 minutes.
- Avoid alcohol before measurement.
- Measure before meals when possible.
- Small habit changes can greatly improve consistency.
Tips for Accurate Monitoring at Home
1. Create a Simple Measurement Routine
Accuracy improves when monitoring becomes part of a steady routine rather than a rushed task.
Choose a quiet place, sit comfortably, and follow the same steps each time. This supports long-term healthy living and reduces unnecessary worry.
2. Keep a Written or Digital Log
Relying on memory can distort patterns. Logging readings provides clarity for you and your healthcare provider.
Record:
- Date and time
- Reading values
- Any relevant notes (stress, illness, poor sleep).
- Focus on Trends, Not Isolated Readings
Blood pressure fluctuates naturally. One high reading does not mean failure or danger.
Looking at weekly or monthly trends provides a more accurate picture of cardiovascular health and helps maintain emotional balance.
3. Use Clinically Validated Devices
Not all blood pressure monitors meet medical accuracy standards. Cheap or unverified devices increase the risk of error.
Choose monitors validated by recognized medical organizations and suited to your arm size and needs. Reliable devices form the foundation of trustworthy home monitoring.
4. Review Technique Periodically
Even experienced users develop habits that reduce accuracy over time. Reviewing technique ensures continued reliability.
Revisit:
- Posture
- Cuff placement
- Timing
- Stillness.
When Blood Pressure Monitor Problems Should Not Be Ignored
If readings remain inconsistent despite correct technique, the issue may not be the monitor. It may signal an underlying health concern.
Seek professional guidance if:
- Readings vary widely without explanation.
- Symptoms like dizziness or chest discomfort appear.
- Home readings differ greatly from clinic readings.
- Accurate monitoring supports informed care, not self-diagnosis.
Final Thoughts on Blood Pressure Monitor Problems
When you use blood pressure monitors the right way, they become really useful. Most problems with these devices aren’t because they’re broken; it’s usually because people make mistakes. If you know what you’re doing wrong and fix it, you’ll trust your readings more. This can make checking your blood pressure a regular and enjoyable habit that helps you stay healthy.
Getting accurate numbers leads to better choices, improved moods, and clearer talks with your doctor. When done correctly, monitoring helps you stay aware instead of stressed out.
Home and selfcare
Portable vs. Tabletop Nebulizers: Which is Better for Home Use
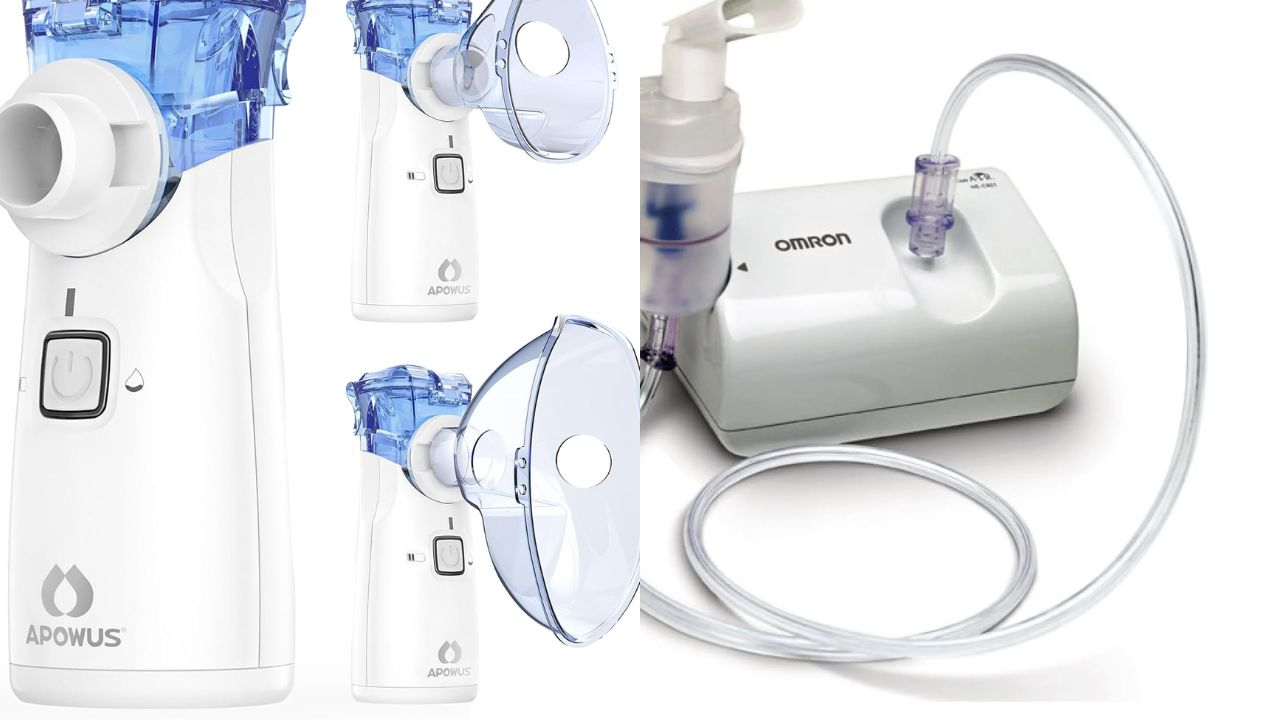
The portable vs tabletop nebulizers question comes up a lot, especially if you or someone you care about uses one for asthma, COPD, or respiratory condition. The right nebulizer should focus on comfort and reliability. Portable and tabletop nebulizers both deliver medicine to the lungs, but they’re made for different needs.
You’ll learn how tabletop and portable nebulizers differ, how each one works, what features to expect, and what to consider before choosing one for home use. The goal is simple: help you make a choice that supports better breathing and long-term health.
What is a Nebulizer
A nebulizer is a device that converts liquid medicine into a mist that can be breathed in through a mask or mouthpiece. It is used for the treatment of respiratory diseases such as asthma, chronic obstructive pulmonary disease (COPD), and bronchitis, or for any other condition that causes difficulty in breathing.
Nebulizers enable the drugs to go deep into the airways, which can ease symptoms such as wheezing, shortness of breath, and inflammation.
With inhalers, you get one quick puff of medicine; with a nebulizer, you get a steady mist of medicine for a few minutes, which makes it easier to use for children, the elderly, or those who have trouble using inhalers correctly.
There are two categories of nebulizers for home use: a tabletop model, which is larger and plugs into a power outlet, and a portable nebulizer, which is compact, battery-powered, and built for mobility.
Portable vs Tabletop Nebulizers
When you want to choose between a portable and a tabletop nebulizer, focus on how each will fit into daily life. Both turn liquid medication into a breathable mist, but they differ in how they deliver that mist, their size, and their power sources. Before looking at features, you should also understand the difference
What Is the Difference Between a Tabletop and Portable Nebulizer?
The main differences are size, power source, and mobility.
- A tabletop nebulizer is larger and meant to stay in one spot, usually on a table or bedside stand.
- It plugs into an outlet and uses a compressor to create steady airflow.
- You’ll see these often in homes, clinics, and hospitals.
For portable nebulizer machine:
- A portable nebulizer is compact and lightweight, designed to be carried around.
- It usually runs on rechargeable batteries or AA batteries.
- It uses mesh or ultrasonic technology instead of a compressor.
Both types can deliver medication effectively, but their designs affect noise level, treatment time, maintenance, and overall convenience.
Tabletop Nebulizers for Home Use

What to Know About Tabletop Nebulizers
Tabletop nebulizers have been used for decades and remain a trusted option for home respiratory care. Doctors often recommend this treatment for patients who require ongoing medication throughout their entire treatment duration.
How Tabletop Nebulizers Work
Most tabletop nebulizers use compressor technology. The machine pushes air through tubing into a nebulizer cup, where liquid medication is turned into a fine mist. Patients use mouthpieces or masks to inhale the generated mist.
This method functions effectively with multiple types of drug treatments.
Tabletop Nebulizers Basic Functions:
Tabletop nebulizers produce unchanging airflow, which guarantees complete medication delivery to patients. This feature becomes essential for patients who experience moderate to severe breathing problems because they require consistent medication delivery.
Wide Medication Compatibility
These devices work with most prescribed nebulizer medications, including thicker solutions. This makes them a safe choice when medication requirements may change over time.
Durable Design
Tabletop nebulizers are built for daily use. Many models last for years with proper care, making them a long-term investment for home use.
Pros of Tabletop Nebulizers
- Reliable and powerful performance
- Suitable for all age groups, including infants and seniors
- Compatible with most medications
- Often covered by insurance when prescribed.
Cons of Tabletop Nebulizers
- Somehow big
- Require a power outlet
- Can be noisy compared to portable models.
Who needs a tabletop nebulizer?
A tabletop nebulizer is better for home use if you:
- You have daily nebulizer treatments.
- You prefer a more stable, stay-at-home environment.
- You are taking drugs that require large volumes of airflow.
- You are not concerned with the white noise.
For many families, a tabletop nebulizer is still the most reliable option.
Portable Nebulizers for Home Use

Portable nebulizers are built for adaptability. They are great for individuals who need their treatments to fit in with a busy or on-the-go lifestyle.
How Portable Nebulizers Work
Some portable nebulizers use mesh technology, and some use ultrasonic vibration. A vibrating fine mesh with tiny holes pushes the medication through, creating a mist. The architecture permits the device to be compact, silent, and battery-driven.
Key Features of Portable Nebulizers
Compact and Lightweight
Portable nebulizers are small enough to be carried in a purse or pocket. This makes them perfect for storage and for travel and home use.
Battery-Powered Convenience
Several models on the market are battery rechargeable for treatment without an outlet, so check these out based on your needs and budget. It’s great for when you experience a power outage or when you lug it from one room to the next.
Quiet Operation
Compared with table-top nebulizers, portable models are far quieter. This is a huge advantage for use at night or for children who are sensitive to noise.
Pros of Portable Nebulizers
- Easy to carry and store
- Quiet and discreet
- Good for traveling or a busy home.
- Useful in different positions.
Cons of Portable Nebulizers
- Lesser capacity for medication
- Must be charged regularly or have their batteries replaced
- Mesh components require a sensitive cleaning.
Who Should Buy a Portable Nebulizer?
You need it if:
- You are often traveling or on the road.
- You’re sensitive to noise
- You need very occasional or brief treatments.
Portable vs Tabletop Nebulizers: Their Features
Power Source and Dependability
Tabletop nebulizers run on electricity, so they offer a steady performance, although you have to use them in a certain area. Portables use batteries, which you need to recharge. Tabletop models often just seem more trustworthy for day-to-day therapy without interruption.
Treatment Time and Efficiency
The tabletop nebulizers has stronger airflow which means faster delivery . Portable nebulizers may take a bit longer, depending on the model and type of medication you have. This difference will matter to those who need fast, efficient sessions.
Noise Level
This is one of the main differences between portable and tabletop nebulizers. Portable nebulizers are far quieter than their tabletop equivalents, which rely on compressor motors for power. Portable models are much quieter, and I can imagine that would make for better comfort and perhaps even compliance.
Maintenance
Both are to be cleaned regularly, but portable nebulizers particularly mesh ones require a bit more handling, so be gentle. Mesh parts may clog if they are not washed properly. Tabletop nebulizers, in general, are tougher and easier to maintain over time.
How Your Lifestyle Influences Your Choice of Nebulizer
- Lifestyle Active: When you hustle in and out of the rooms of your house or out on the road, a portable nebulizer makes treatment more manageable and ensures that you never miss a dose.
- Fixed Routine: If you have your treatments in one place, such as a bedside table, a tabletop nebulizer offers more powerful airflow, quicker sessions, and consistent quality.
Choosing the Best Nebulizer for Your Day-to-Day Needs
- Treatments in the Morning and Evening: You can use these models early in the morning or late at night without waking up anyone, as they are quiet.
- Several Users in a Household: Tabletop nebulizers are very suitable to be shared since they normally come with bigger medication cups and are easy to use.
- Senior or Kid-Friendly Operation: Tabletop models tend to have larger, more legible buttons, and portable ones include the need to handle the mesh parts with care.
Safe and Effective Medication Delivery
Both handheld and tabletop nebulizers can provide the right dose when properly used. The important thing is to follow the manufacturer’s guidelines and maintain the device.
Tabletop nebulizers are well-established in clinical practice—this reassures some users. Portable nebulizers have come a long way in the last few years and are now deemed safe for home use by regulatory agencies.
Reasoning About Costs for Home Use
Initial Purchase Price
Because of the advanced technology, portable nebulizers sometimes have a higher initial price. Tabletop nebulizers can be more cost-effective and are often partially or fully reimbursed by insurance with a prescription.
Long-Term Expenses
Tabletop nebulizers may also need replacement tubing and masks, which are usually inexpensive. Disposable mesh parts or batteries for portable nebulizers are needed periodically, which might result in additional long-term costs.
Portable vs Tabletop Nebulizers: Which is Better for Home Use
- The right choice depends on how you live and how you treat your respiratory condition. However,
- Go with a tabletop nebulizer if you want power, consistency, and reliability over time at home.
- Get a portable nebulizer if you want more flexibility, want it to be quiet, or want to be mobile.
- Most homes actually have the two. A tabletop nebulizer for everyday medicine and a portable one for an emergency.
Read also: Best Nebulizer Machines for Asthma: Quiet, Fast, and Doctor-Approved Models
FAQs
1. What is the difference between a tabletop and portable nebulizer?
A tabletop nebulizer uses electricity, is bigger, and remains stationary, whereas a portable nebulizer is a small, battery-powered device that you can take with you wherever you go. Both deliver medication effectively.
2. What is the best nebulizer for home use?
It depends on your routine. For daily treatments that take place in a fixed location, a tabletop nebulizer is the best choice. Quiet, portable nebulizers work great for use at home.
3. Can portable nebulizers handle all types of medications?
Not always. Some portable mesh models may not work with thicker medications. Tabletop nebulizers generally support a wider range of prescriptions.
4. Are portable nebulizers as effective as tabletop ones?
Yes, if used properly. Portable nebulizers deliver accurate doses, but treatment time may be slightly longer compared to tabletop models.
5. How do I clean and maintain my nebulizer at home?
Rinse the medication cup, mask, or mouthpiece after each use. Tabletop models are easier to clean, while portable mesh devices need careful handling to prevent clogs.
Final Thoughts on Portable vs Tabletop Nebulizers
In the portable vs tabletop nebulizer debate, the right choice is the one that you will use the most. More effective is one that matches your routines, comfort level, and medical requirements.
Knowing the difference between a tabletop and portable nebulizer will enable you to get rid of the marketing hype and concentrate on what really matters for better breathing.
-

 Diagnostic & Hospital Equipments4 months ago
Diagnostic & Hospital Equipments4 months agoWhat Are Medical Devices? Types and Uses
-

 Uncategorized4 months ago
Uncategorized4 months ago6 Best Heatmap Plugins – I Test, Review and Compare
-

 AI in Health care4 months ago
AI in Health care4 months agoRemote Patient Monitoring in Modern Healthcare
-

 AI in Health care1 month ago
AI in Health care1 month agoDigital X-ray vs. Film X-ray: Which is better?
-
 Review and guides3 months ago
Review and guides3 months agoCPAP Machines Buying Guide: The Best Models Doctors Don’t Recommend
-

 AI in Health care4 months ago
AI in Health care4 months agoAI in Medical Imaging: What is Coming Next
-
 Diagnostic & Hospital Equipments1 month ago
Diagnostic & Hospital Equipments1 month agoDEXA Bone Density Scanning: What You Need to Know About Bone Health
-
 Diagnostic & Hospital Equipments1 month ago
Diagnostic & Hospital Equipments1 month agoPET Scan Machines: Understanding the Technology, and Usage
