Diagnostic & Hospital Equipments
MRI Machine vs. CT Scan: Which Imaging System Should Your Facility Invest In?
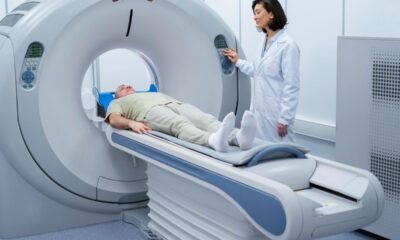
When a hospital or diagnostic center wants to remodel its imaging department, the question often is, MRI machine vs CT scan: which makes more sense for them? Doctors use both machines to scan the body without performing surgery. With these machines, they can detect injuries, tumors, infections, and bleeding in the body. However, they work differently.
You’re probably asking what a CT scan can detect that an MRI can’t. Which one has better resolution for the brain? And how much is each system?
Let’s not forget the patient experience. Some people get nervous while having an MRI because the machine is so small and can make them feel claustrophobic. Some with anxiety have trouble with MRI scans. CT scanners are more open and they are faster.
So this is not just a question of technology. Budget, the number of patients, and the types of diagnoses are all important. In this article, we will explain the difference between CT scans and MRIs, the type of images they produce.
What is the difference between a CT scan and an MRI?
To select the most suitable imaging system, it is vital to know the basic principles of each system.
A CT scan, also known as a computed tomography scan, involves X-rays processed by a computer. The device revolves around the patient and takes several X-ray pictures. Afterwards, the computer processes the images and produces cross-sectional images of the body.
An MRI (magnetic resonance imaging) scanner is different. It depends on strong magnets and radio waves instead of radiation. The device detects how hydrogen atoms in your body behave in magnetic fields. Those signals are processed into high-resolution, detailed images.
So if you are asked about the difference between CT scans and MRIs, the answer is technology. A CT scan is a modality that involves radiation and imaging similar to an X-ray. MRI operates by using radiofrequency signals and magnetic fields.
This one difference informs everything else: the kinds of diseases each scan can detect, how quickly images can be obtained, patient safety issues, and the cost of installation.
CT scans are faster. Doctors prefer them in emergencies. They take longer, but they give a far more detailed view of soft tissue. Knowing even this one fundamental difference can help you with your decision-making.
What Does a CT Scan Show?
CT scans show structures where there is a difference in density. Bones, bleeding, lung tissue, and internal trauma can be seen well on CT images. When to get a CT scan, your doctor may recommend a CT scan if they suspect:
- Internal bleeding
- Bone fractures
- Lung infections
- Cancer spread
- Organ injuries
- Blood clots in the lungs.
If a patient arrives at the emergency room after a car accident, the CT scanner is the first imaging tool to be used. The machine can capture full-body images in just a few minutes.
A CT scan performs well when imaging the brain during acute conditions. If doctors suspect a stroke caused by bleeding, CT imaging can detect it quickly. This allows physicians to make rapid treatment decisions.
For facilities that treat trauma cases, emergency medicine, or acute neurological conditions, CT scanners provide immediate clinical value.
What Does an MRI Show Better?
MRI machines excel at visualizing soft tissues. These tissues include muscles, ligaments, nerves, cartilage, and internal organs.
MRI scans help doctors diagnose the following conditions:
- Torn ligaments
- Spinal cord injuries
- Brain tumors
- Multiple sclerosis
- Joint abnormalities
- Soft tissue cancers.
When more detailed images of the brain are required, MRI can identify subtle changes in brain that CT scans do not see.
MRI also enables healthcare professionals to detect inflammation, nerve damage, and small structural changes.
This is why MRI is so useful in neurology, orthopedics, and oncology.
MRI vs CT Scan Images: Their Similarities
The images produced by CT and MRI scans look very different.
CT images resemble highly detailed X-rays. They show bones, blood, and organs with clear contrast between dense and less dense structures. Physicians can also reconstruct these images into three-dimensional models.
MRI images look more detailed when examining soft tissues. The contrast between muscles, nerves, and connective tissue appears sharper. This helps doctors identify small abnormalities.
For example, a ligament tear in the knee appears clearly on MRI images. A skull fracture, however, appears more clearly on CT images. Both technologies generate cross-sectional slices of the body, but the level of soft tissue detail differs significantly.
Because of this difference, many hospitals use both systems. They complement each other instead of replacing each other. But if a facility must choose only one, the decision depends on the patient population.
Brain Imaging: MRI vs CT Scan
Neuroimaging is arguably one of the most salient contrasts between these two modalities. They can both produce images of the brain’s structures, although they are used in different clinical contexts. A CT scan is usually the first-line option for emergency brain imaging.
During emergencies such as stroke or traumatic brain injury, speed is necessary. MRI, however, have a higher-resolution image of the brain. They detect tissue damage that is not readily apparent (for example, tumors, nerve disorders, and degenerative diseases). Neurologists use MRI scans to help diagnose:
- Brain tumors
- Multiple sclerosis
- Brain infections
- Chronic neurological diseases
So when deciding between an MRI machine and a CT scan, facilities must consider the type of brain conditions they expect to diagnose.
CT Scan Cost vs. MRI Cost
A CT scanner costs between $300,000 and $2 million, depending on the model and imaging capability.
MRI machines usually cost $1 million to $3 million or more. High-field MRI systems can exceed that range.
MRI machines require specialized rooms with magnetic shielding. The building must support heavy equipment and magnetic safety zones. Facilities may need structural modifications before installation.
CT scanners require less complex infrastructure. The system still needs radiation shielding, but installation usually costs less.
MRI machines require cryogenic cooling systems and magnet servicing.
Imaging Speed: Why It Counts
A CT scan take less than five minutes. The procedure can last only seconds.
MRI exams can take from 20 to 45 minutes, depending on the body part.
CT scanners are able to handle more patients in one day. This speed is vital for emergency departments. While MRI scans provide deeper diagnostic information, they are slower. Detailed soft tissue imaging scans can be longer.
MRI machines are uncomfortable for some patients, in particular those who are claustrophobic. Within a short time, a patient is lying inside a tube surrounded by magnets. The scan also makes loud banging noises while imaging. Some patients become nervous during the operation.
This is accomplished by using more comfortable and wider bores and by quieter scan technology on modern MRI systems. However, even so, it can feel restrictive for some patients. CT scanners feel more open. The patient passes through a compact doughnut-shaped struture, as opposed to a lengthy tube in traditional systems.
Radiation Exposure: Safety Consideration
Radiation is another big distinction between CT scans and MRIs.
CT scans are performed with X-ray radiation. Although the level of exposure is considered safe. This is why doctors have weigh carefully whether a CT scan is necessary before they order one.
MRI machines don’t depend on ionizing radiation. They use magnetic fields and radio waves. This aspect also makes MRI the preferred modality for serial imaging studies, in pediatric patients.
The potential of frequent follow-up imaging of chronic conditions is something that would make MRI appeal to any center. Nonetheless, there are still contraindications to MRI for some patients with certain implants or metal devices.
Space and Installation Requirements
- Because MRI machines are so heavy, the system also needs a strong floor support.
- CT scanners also need their own imaging rooms, although the building requirements tend to be less complex.
- CT installation is somehow easier and faster if your facility is small
Clinical Demand: What Do Your Patients Need?
The biggest challenge in deciding between MRI and CT technology is patient demand.
Note the types of cases your facility handles most frequently.
ERs and trauma centers need lots of CTs.
MRI, meanwhile, is mostly used by orthopedic clinics to assess ligaments and joints.
Neurology centers with sophisticated brain imaging focus more on MRI.
Both technologies can be used in cancer screening programs.
Revenue Potential for Imaging Services
Imaging equipment also functions as a revenue generator for healthcare facilities.
CT scans cost less for patients. Insurance providers often reimburse them at lower rates.
MRI scans cost more because of the advanced technology in it.
However, MRI exams take longer. That means fewer scans per day compared to CT.
A CT scanner may process more patients daily, creating steady imaging revenue.
MRI systems may generate higher revenue per scan but lower volume daily.
When a CT Scan Is the Better Investment
A CT scanner may be the better choice when a facility needs the following:
- Fast emergency imaging
- High patient throughput
- Lower installation cost
- Trauma and injury diagnosis
- Lung and chest imaging
When MRI is the Better Investment
MRI systems may be a better choice when facilities focus on:
- Neurology diagnostics
- Soft tissue imaging
- Orthopedic evaluation
- Cancer detection
- Advanced brain imaging
MRI offers deeper diagnostic insights for complex conditions.
Specialized clinics often rely heavily on MRI for accurate diagnosis.
Facilities that market advanced imaging services may benefit more from MRI technology.
Should Your Facility Invest in Both?
Many modern hospitals choose not to compare MRIs vs. CTs as competitors. Instead, they treat them as complementary tools.
- Each technology solves different diagnostic challenges.
- A CT scanner may serve emergency care and trauma imaging.
- An MRI system may handle neurological and musculoskeletal imaging.
- Facilities that invest in both technologies provide broader diagnostic services.
- This approach increases clinical capability and improves patient care.
- However, smaller diagnostic centers may start with one system and expand later.
Questions to Ask Before Choosing an Imaging System
Before you buy an imaging equipment, these questions are necessary:
- What conditions do we diagnose most often?
- Do we treat emergency cases regularly?
- What imaging services do referring physicians request?
- How much installation space do we have?
- What is the cost of equipment?
Read also: DIY Health Monitoring: What’s Worth It and What Could Cost You
Final Thoughts: MRI Machine vs CT Scan
So what should your facility buy: an MRI machine or a CT scan? It all depends on the requirements for clinical use, the demand from the patients, and how much money is available.
CT provides rapid acquisition of images, excellent performance in an emergency setting, and lower cost for installation. They are also very efficient for trauma, lungs acute brain disorders.
MRI provides more detailed information on soft tissue, nerves, and intricate neurological conditions. These systems produce high-resolution images that can be used to identify even the finest abnormalities.
Complement each other. Some healthcare facilities acquire both types of machinery, which complement each other. However, if you need to buy only one for your facility, focus on the patient’s needs.
Diagnostic & Hospital Equipments
Best C-Arm Imaging Machines for Operating Rooms
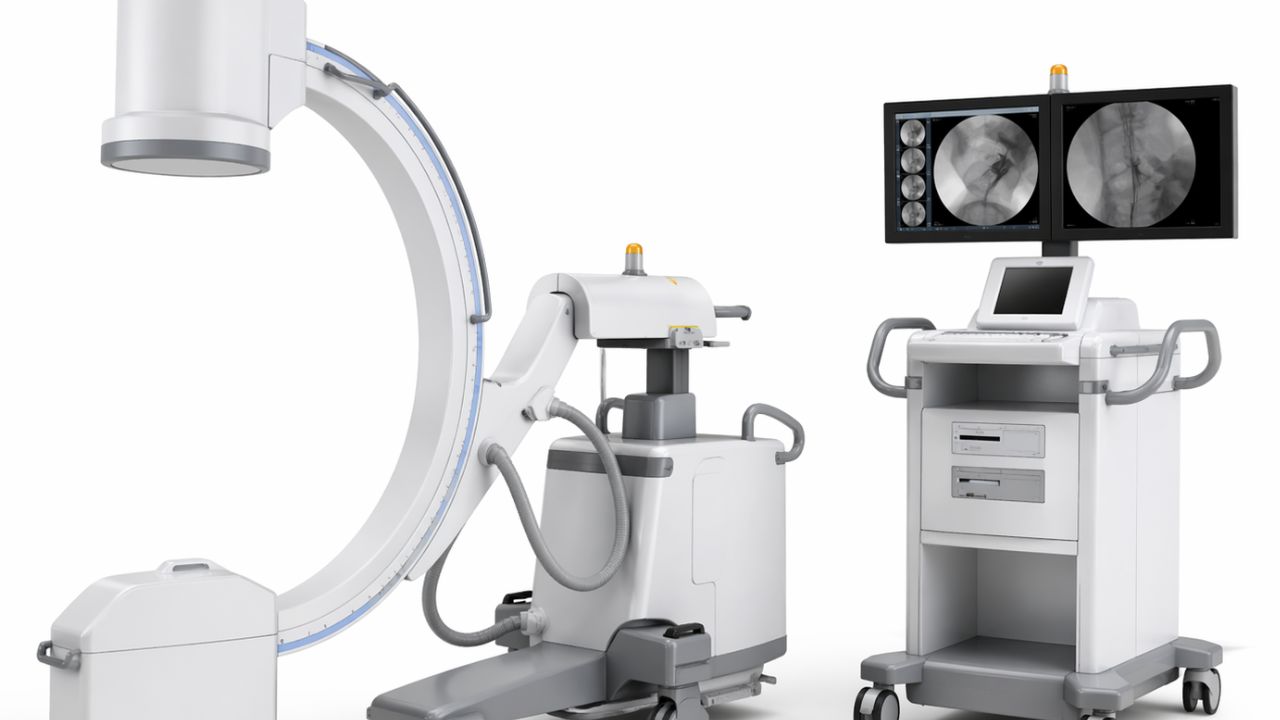
C-arm imaging machines for operating rooms need to balance surgical accuracy and budget. C-arms are part of modern fluoroscopy, as they provide real-time X-ray assistance during complex procedures. When choosing the right machine, look for high-resolution imaging that limits radiation exposure and keeps maintenance costs low.
Whether you want advanced 3D imaging for orthopedic operations or an affordable model for general surgeries, there are numerous options on the market.
In an operating room, you may see a piece of equipment that looks like a giant, metallic letter “C” on wheels. It’s a C-arm machine. A C-arm is a mobile X-ray unit that allows surgeons to see “live” images of the inside of your body while they perform the procedure.
Why Is It Called a “C-Arm Machine”?
The name of the machine is quite apt: it features an arm that connects an X-ray source and an X-ray detector. The arm is shaped like a “C,” so it rotates easily around the patient. This means doctors can get images from almost any angle without having to get up and change the patient on the operating table.
What Is a C-Arm Machine Used For?
In the past, surgeries often required large, invasive cuts because doctors had to see what they were cutting. But today, with C-Arm technology, surgeons can carry out “minimally invasive” procedures.
Here are the most common ways this tool is used:
Orthopedic Surgeries (Bone Repairs)
When treating a bone fracture and need to fix it with rods, plates, or screws, a C-arm can be an excellent tool for the surgeon. It can scan in real time and allow the surgeon to place the hardware precisely and correctly before ending the procedure.
Pain Management Injections
People with chronic back or neck pain go to the clinic for targeted injections. The doctors use the C-arm to guide the needle to the exact spot on the spine to ensure that it gets to the right place.
Cardiac and Vascular Procedures
C-arms are an important tool in cardiac and vascular operations. It passes a contrast dye into the blood, and it can identify and treat blockages or to place stents.
Pacemaker Implantation
For those who need a pacemaker, the doctor must direct fine wires through the veins.
What are the 7 types of Imaging?
In addition to the C-arm, health practitioners also use a variety of imaging devices to scan inside the body. Here are the most common imaging techniques.
X-Ray (Radiography)
Most commonly used, this method uses a small amount of radiation to create a two-dimensional image. This is used to detect fractures, dental cavities, or pneumonia.
Computed Tomography (CT Scan)
Using a CT scan, radiologists take multiple X-rays from different angles. Computers assemble these images into “slices” of the body. This gives doctors a clearer view of organs and tissues than with an X-ray.
Magnetic Resonance Imaging (MRI)
MRI technology doesn’t rely on radiation. Instead, it uses powerful magnets and radio waves to produce body maps. It is considered the best method for examining soft tissues, such as the brain, spinal cord, muscles, and ligaments.
Ultrasound (Sonography)
Ultrasound uses high-frequency sound waves to generate images. It is entirely safe and free from radiation, which is why it is the preferred option for monitoring pregnancies and assessing blood flow in veins.
PET Scan (Positron Emission Tomography)
A PET scan involves a radioactive tracer to visualize the functionality of your body’s tissues, rather than just their appearance. Physicians often use this technique to monitor diseases like cancer or evaluate heart health.
Fluoroscopy
This device is used for fluoroscopy, which acts like a live X-ray film. It enables doctors to observe joint movement or track the flow of liquids (such as contrast dye) through the digestive system in real-time.
Nuclear Medicine
Nuclear medicine involves introducing a small amount of radioactive material into the body to emphasize certain areas. It detects early signs of disease in bones or organs that other imaging methods may overlook.
How much do C-Arm Imaging Machines Cost?
Prices are not always available and may require you contact suppliers for a quote. So, what’s the cost of a C-arm machine? Prices range from $20,000 to over $250,000. We’ll consider these things:
1. New vs. Refurbished
New C-Arms ($100,000 – $250,000+): Opting for a new model ensures you receive the latest Flat Panel Detector (FPD) technology, a comprehensive manufacturer warranty, and the longest operating life. For intricate vascular or cardiac procedures, a new machine is better.
2. Refurbished C-Arms ($35,000 – $90,000)
High-quality refurbished models from brands like OEC or Siemens can match new units’ performance at half the cost. It’s vital to buy from a reliable vendor with a strong warranty.
3. Used/As-Is C-Arms ($20,000 – $35,000)
This option carries risks. Initial savings might seem attractive, but an unexpected failure, such as a faulty image intensifier, could require a $15,000 part replacement soon after buying.
Types of C-Arm Technology
Image Intensifiers vs. Flat Panel Detectors
Traditional C-arms come with image intensifiers, recognizable by their large bell-like shape. They are dependable and economical.
Modern C-arms, however, feature flat panel detectors, have higher resolution, and are durable.
C-Arm Sizes and Applications
The type of surgery will dictate the C-arm size to get. For example:
Mini C-Arms
($30k – $70k): Ideal for treating hands, feet, and extremities, making them perfect for orthopedic practices.
Full-Size C-Arms
($50k – $150k): Versatile and suitable for spine, pain management, and general surgeries.
Vascular/Cardiac C-Arms
($100k+) Designed for high-power operations (with 30kW generators) and equipped with sophisticated software for vascular imaging, these are the priciest models available.
C-Arm Imaging Machines: Top 4 Brands
Below are some of the leading C-arm models in 2026.
OEC Elite CFD (GE Healthcare) C-Arm Imaging Machines
Renowned for its status in surgical imaging, the OEC Elite is one of the most used by surgeons.
- Feature: High-definition CMOS flat panel detector.
- Advantage: Delivers sharp images and still reduces radiation exposure relative to older systems.
- Benefit: Enables your team to handle complex procedures in orthopedics, vascular, and cardiology. It reduces the risk of repeat operations and enhances patients’ safety.
Ziehm Vision RFD (Ziehm Imaging)
For facilities focused on intricate vascular surgeries, the Ziehm Vision RFD supports your operational needs.
- Feature: Robust 25kW liquid-cooled generator.
- Advantage: Supports lengthy and demanding surgeries without overheating or lessening image clarity.
- Benefit: Minimizes downtime for machine cooling, allows more time for patient care, and boosts your surgical efficiency.
Philips Zenition 70
Philips emphasizes “Unified User Experience.” It makes sure that the machine is highly user-friendly for your team.
- Feature: Tablet-like touchscreen interface.
- Advantage: The intuitive software simplifies learning and controls.
- Benefit: Cuts down on training time and prevents technical delays. Keeps your surgical team efficient and focused.
Siemens Healthineers Cios Spin
For surgeons that specializes on spinal or trauma surgeries, the Siemens Healthineers is recommended.
- Feature: Complete 3D navigation and in-surgery CT-like imaging.
- Advantage: Allows real-time verification of implant placements right in the OR.
- Benefit: Lowers the necessity for additional surgeries. Save money and enhance patients’ recovery.
How to Choose the Right C-Arm Machines for Your Facility
Consider these questions:
- What is the main focus of my practice? (Orthopedics, Vascular, Pain Management, or General Surgery?)
- Is image quality my priority? (Think about CMOS flat panel detectors.)
- How much floor space is available? (Some models are for smaller clinics.)
When investing in brands like GE, Ziehm, Philips, or Siemens, you’re securing the following:
- Reliable Uptime: Reducing calls for repairs.
- Advanced Radiation Safety: Ensure the well-being of both your staff and patients.
- High Resale Value: These models maintain their value longer compared to cheaper alternatives.
The Factors to Consider:
1. Image Quality: Flat Panel vs. Image Intensifier
Before, C-arms were equipped with image intensifiers (II), known for their large, drum-like appearance. These devices are dependable and cost-effective, but they use older technology. Nowadays, many modern medical facilities prefer Flat Panel Detectors (FPD) for the following reasons:
- Zero Distortion: Flat panels deliver clear, square images without the “fisheye” effect associated with outdated models.
- Reduced Radiation: These detectors need a lower radiation dose to yield high-quality images.
- Streamlined Design: Being flat, they are easier to position around patients and surgical tables.
2. Power and Generator Capacity
C-arm machines have different power capacity like:
- 15kW to 25kW Generators: Suitable for intensive tasks such as vascular, cardiac, or bariatric procedures.
- 2.5kW to 7.5kW Generators: Optimal for orthopedic surgery, hand operations, or pain management.
3. Mobility and Space Efficiency
Consider the space in your hospital. Before you buy, think of these factors below:
- Does it have a rotating anode?
- What is its lateral travel capacity?
- Is it easy to move in tight spaces?
4. Refurbished vs. New Equipment
Buying a certified refurbished C-Arm from a trusted dealer can save between 30% and 50% of the cost of a new unit. However, for used devices, ensure the dealer offers a warranty and detailed tube life records.
5. Software Compatibility and Connectivity
Your C-Arm interfaces should be able to connect with your office systems easily. Confirm that the device is DICOM compatible for image transfer to PACS systems or printers.
Comparison Table: C-Arm Imaging Machines
| Machine Type | Price Range | Key Feature | Best Use Case |
| Compact C-Arm | $25k – $50k | Small footprint | Pain clinics & podiatry |
| Standard C-Arm | $50k – $100k | Versatile imaging | Orthopedic surgery |
| Premium 3D C-Arm | $150k – $300k | Volumetric imaging | Spine & vascular surgery |
Final Thoughts About C-Arm Imaging Machines
Hospitals and surgical centers use C-arm imaging machines to deliver high-resolution, real-time X-ray images during major operations.
From orthopedic operations to cardiac interventions, surgeons depend on C-Arms for precise instrument guidance while the patient is on the operating table.
Whether you opt for a new model or a certified pre-owned unit, the right selection will improve your surgical capabilities and patient results. Do you have further questions about how these machines operate? Feel free to ask in the comment section!
Disclaimer: This guide is for informational purposes only. Consult your surgical team before you buy any medical equipment.
Diagnostic & Hospital Equipments
Hospital Ventilation Systems: Recommended Machines

The hospital ventilation systems are not for temperature control only. They regulate airflow, air pressure, and airway pressure to ensure that the air patients, staff, and visitors breathe is healthy. So, when a hospital’s ventilation is doing its job, it’s quietly working to keep things clean and help everyone get better faster and safer.
The hospital constantly receives a steady flow of visitors and staff. Such activity creates a toxic environment where germs, odors, and airborne contaminants can breed rapidly and spread easily, increasing the risk of infection to everyone present.
Understanding Hospital HVAC Systems
Clinic HVAC systems are more complex than the traditional air conditioning units. A key element in these systems is the management of pressure differences, which control air movement inside the building.
By carefully regulating air pressure, it can suppress the spread of disease. Positive pressure settings are used in sensitive areas like operating rooms or burn units to keep germs out.
In this case, slightly increasing the pressure allows clean air to flow outside when the doors open, preventing contaminated air from entering the corridor. However, negative-pressure rooms are designed to contain germs.
These are found in isolation or tuberculosis wards, where the pressure is set lower than in the surrounding spaces, ensuring that air is drawn into the room when doors open and containing the potential.
While an ordinary room may only require minimal air changes per hour, hospitals demand high air exchange rates (ACH) to dilute and remove pollutants. This frequent turnover of air prevents stagnation, which is crucial, given the concentration of pathogens in medical settings.
Also, the air quality is maintained using advanced filtration systems. Ordinary furnace filters are inefficient in these environments; instead, health centers use MERV-rated and hospital-grade HEPA (High-Efficiency Particulate Air) filters. HEPA filters are the industry standard, capable of capturing at least 99.97% of dust, pollen, mold, bacteria, and particles as tiny as 0.3 microns.
Critical Zones: The Importance of Airflow
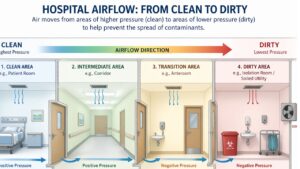
In a hospital setting, ventilation is needed for the safety of everyone present. Special areas of a hospital or medical facility are called critical zones. These areas are airtight to germs and pathogens.
Operating Rooms
Operating rooms are among the most delicate areas. To maintain sterility and minimize exposure to dust and bacteria, these rooms employ a technique known as laminar flow. This system directs a continuous, smooth stream of clean, filtered air over the patient, functioning as an invisible barrier to keep potential contaminants away from the sterile field.
Intensive Care Units (ICUs)
In Intensive Care Units (ICUs), the need for ventilation is different: care providers are asked to provide comfort and prevent infection while maintaining patient safety. Patients in these units have compromised immune systems. Ventilation in these units should be strong enough to eliminate pathogens from the air while still providing a stable environment for the patient’s recovery.
Isolation Rooms
An isolation room is equipped with separate exhausts that collect air and prevent it from traveling out into the hospital corridors. Since the air pressure inside the room is lower than in the rest of the hospital, any air contaminants are confined to the room and safely ventilated outside so they do not return to the hospital.
Laboratories and Pharmacies
These areas can handle flammables, hazardous substances, and even sensitive medications. Ventilation systems constantly refresh the air to keep dangerous fumes out.
This is why hospitals need quality ventilation systems. These ventilators can control air humidity and remove bacteria and viruses from the air, as well as harmful gases and dust from the air.
Pressure differences can also be used to avoid cross-contamination between rooms. When properly designed, these systems can ensure safe operating rooms and isolated isolation rooms for healthcare workers.
Hospital Ventilation Systems: The Top-rated Machines
When it comes to mechanical ventilators, or equipment that assists a patient in breathing, reliability is key. Here are some of the best operating room ventilators.
Hamilton Medical: Hamilton-C6
As a Swiss manufacturer, Hamilton Medical is known for its “intelligent” ventilation solutions. The Hamilton-C6 is considered a standard of advanced care.
- Features: It uses ASV (Adaptive Support Ventilation) that adjusts the patient’s breath rate and pressure based on his or her lung function. It also has a high-flow oxygen therapy mode.
- Use: This ventilator is used in Intensive Care Units (ICUs) for critically ill patients who require advanced, automated respiratory support.
Dräger: Evita V800
Celebrated for its medical technology, Dräger’s Evita V800 is a favorite among respiratory therapists.
- Features: It includes an easy-to-use touch screen and a “Lung Protection Package” to protect against lung damage by preventing excessive pressure. The battery life allows long travel inside or outside the hospital.
- Applications: Used in ICUs in adults and children receiving prolonged mechanical ventilation.
Philips: V60 Plus
Philips is one of the world’s largest companies in medical device manufacturing. Their V60 Plus is a multifunctional device marketed for non-invasive ventilation (NIV).
- Features: The Auto-Trak technology is a highlight; it helps the machine recognize the breaths of a patient. By so doing, it reduces the patient’s effort. It is available in an invasive and noninvasive option. The versatility makes hospitals go for it.
- Use: Ideal for emergency and intermediate care units. Also, it supports patients without the need to intubate the throat.
GE Healthcare: Engström Carestation
GE Healthcare is an organization whose goal is to convert the complexities of data into logical steps.
- Features: The Engström is an innovative “multitool” that can combine ventilation with gas monitoring, and it also has the “neonatal” mode that is ideal for the most delicate or small patients.
- Use: Suitable for busy hospitals. It can be used on preemies and older adults.
Tackling Current Challenges on Hospital Ventilation Systems
- Post-Pandemic Transition: The impact of COVID-19 on the design standards for pandemic-ready medical facilities.
- Balancing Energy Efficiency and Infection Control: The issue of high energy use in hospitals and how smart building management systems (BMS) can help.
- Humidity Management: Why a humidity level of 40%-60% is needed to control the growth of mold and viral infections.
- Routine Inspections: Testing, adjusting, and balancing (TAB) are so important.
- Preventative Measures: Replace filters and clean air ducts to prevent “sick building syndrome.”
ASHRAE Standards for Hospital Ventilation Systems
Prevention involves frequent and consistent cleaning of ducts and air quality filters. Ignoring these tasks can lead to “sick building syndrome,” wherein unclean, polluted air can lead to headaches, fatigue, and respiratory problems for healthcare workers and patients. Clean components ensure that the system runs efficiently and that the air is clean.
In addition, compliance with regulations is not optional. The industry standard is ASHRAE Standard 170 (Ventilation of Health Care Facilities), which specifies air change rates, pressure relationships, and filtration levels for every room in a hospital.
One of the best ways used in operating rooms is using laminar flow. In a typical room, air swirls around and can spread dust and bacteria. But in a laminar flow room, the air moves steadily upward, usually from the ceiling to the floor. It creates a “clean zone” above the patient and carries any germs that might be present on the site.
For instance, a hospital in the UK with an existing UCV system, The Royal Papworth Hospital, installed an Ultra-Clean Ventilation (UCV) systems when they moved in. They optimized air quality and flow by performing high-efficiency air changes and flow patterns. They had extremely low rates of surgical site infections (SSIs).
It is wise to invest in these systems. Hospitals that use specialized filtering and air paths can reduce the risk of secondary infections and will recover more quickly and pay less over the long run.
Related Post: Top 5 Anesthesia Machines for Hospitals That Deliver Performance
Final Thoughts
Hospital ventilation systems filter air to protect vulnerable patients. They do more than regulate temperature; they protect against airborne infections.
Don’t look at the cost of HVAC systems as a utility expense. Consider the value of investing in high-performance air quality systems, which will make your hospital a safe and healthy place for everyone. However, you should research more before you get any of the machines listed here. Better still, consult with HVAC specialists.
Diagnostic & Hospital Equipments
Top 5 Anesthesia Machines for Hospitals That Deliver Performance
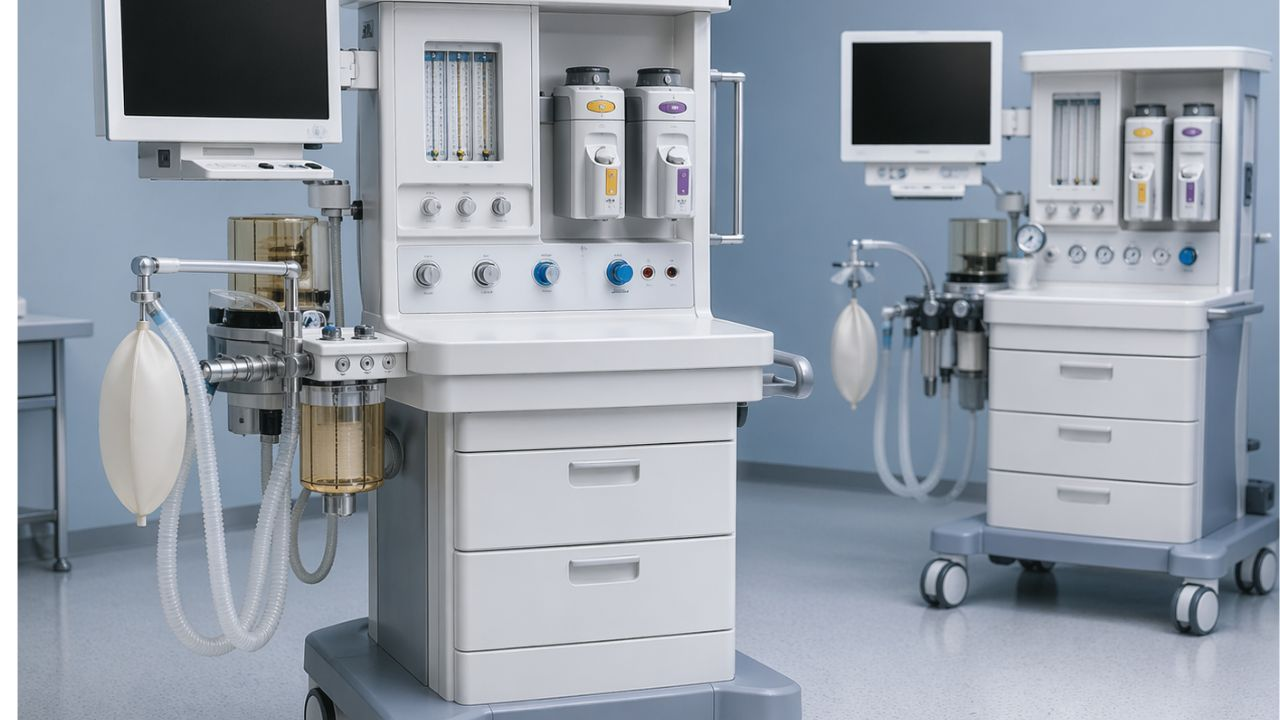
In a busy operating room, the line between a simple surgery and a serious emergency depends on the reliability of equipment and surgeons’ expertise. When a surgeon starts operating, they need tools that will make their job easy, which is exactly what you get with today’s anesthesia machines.
For the anesthesiologist, this machine is key. It’s the link between the patient being awake and them undergoing a pain-free, life-saving procedure. It lets them keep a close eye on the patient’s body functions while the surgeons do their thing.
Every successful surgery is backed by the confidence these machines give. Nowadays, companies make anesthesia machines with advanced breathing and monitoring features.
What is an Anesthesia Machine used for?
Basically, an anesthesia machine mixes oxygen and anesthetic gases to keep the patient asleep and doesn’t feel any pain. It also acts like a breathing machine.
The machine has fancy screens that show things like heart rate, blood pressure, etc. For the anesthesiologist, these numbers are like a way to talk to the patient’s body. If things change, the doctor tweaks the controls. It’s this continuous back-and-forth that keeps the patient in a safe, controlled state of unconsciousness.
What are the 4 types of Anesthesia?
When it comes to surgery and other medical procedures, four main types of anesthesia can be used. They are:
1. General Anesthesia
This type of anesthesia puts a patient into a controlled sleep. The anesthesiologist gives the patient strong medications that stop pain signals from getting to the brain. When the person wakes up, they won’t remember anything about the surgery.
2. Regional Anesthesia
The regional anesthesia numbs a larger part of your body, like the arm, the leg, or the whole lower half. They inject medication near a group of nerves to create a temporary “no feeling” zone for pain. However, an epidural, for example, is injected into the spinal canal and can also be used for childbirth.
With this, the patient can stay awake and chat with the doctor, but your lower body won’t feel a thing during the procedure.
3. Monitored Anesthesia
Often referred to as “twilight sedation,” the monitored anesthesia puts you in a sort of dream-like state. You’re not completely unconscious but relaxed and won’t notice any surgery taking place on your body.
This is mostly used for quick procedures. It’s a nice middle ground between being fully awake and completely asleep.
4. Local Anesthesia
The local anesthesia is the most basic type, used for small surgeries like cuts or biopsies. A numbing liquid (Betadine) is applied to the skin, in the mouth, or injected into the tissue. Local anesthesia is good for procedures that don’t take too long, usually under two hours, such as dental work or taking small tissue samples.
While it’s usually very safe, some people may have reactions like allergies or feel some tingling, burning, or swelling.
Top Anesthesia Machines
Selecting the most suitable anesthesia machine depends on factors such as the hospital’s budget, the clinical requirements, and the preferences of the anesthesiologists. Here are some of the top options available.
GE Healthcare’s Aisys CS2
The Aisys CS2 is a modern version of long-standing operating room machines. Its digital features ensure precise gas delivery and smooth integration with electronic health records.
- Advantage: It has a clean interface and enough ventilation. Also, the parts are easy to get.
- Disadvantage: Expensive due to the high-tech digital features.
- Popular because it’s familiar to those who trained on Ohmeda machines.
Dräger Anesthesia Machines
Dräger’s Perseus A500 is a sophisticated anesthesia machine known for its sleek design and automation. It adapts well to different patient sizes and includes automatic lung recruitment operations.
- Benefit: Saves space
- Advantages: Has a beautiful custom screen layout. Doesn’t make noise and does much of the work for you.
- Disadvantage: Requires software training.
- Popular due to the automation and advanced ventilation options.
Mindray: A9
Mindray used to be considered the “budget” alternative, but the A9 has transformed that notion. It’s not as expensive as the Aisys CS2; however, it serves well.
The benefit is that it serves as a “workhorse,” dependable, and user-friendly.
Key features include a large, easy-to-read touchscreen and an integrated “High-Flow Nasal Cannula” mode.
Advantages: Offers excellent value for the price. You get high-end features (such as improved ventilation).
Disadvantages: The build quality is acceptable, but not durable like previous GE or Dräger units. Some clinicians still need to familiarize themselves with the UI.
Why hospitals like it: For hospitals that desire high-end technology, it is still affordable.
IntelliSave AX700 from Philips
It makes perfect sense that Philips has an anesthesia machine that communicates easily with their monitor systems. The company is famous as a reliable brand for patient monitoring.
- Benefits: If your hospital is already a “Philips shop,” this makes more sense. The flow of data is incomparable.
- Key Features: It’s incredible how it integrates with Philips patient monitors. It lessens the “alarm fatigue” that so many medical professionals experience.
- The Advantages: Unified. Instead of feeling like a machine and a monitor pasted together, it works as a single, coherent system.
- Disadvantages: It is nearly overly integrated. The device may feel a little limiting if you don’t like the Philips ecosystem.
- Popular for: The data storage is the main reason people go for it. This device is perfect for anesthesiologists who enjoy having all their patients’ vital signs and breathing data in a synchronized stream.
Prima 465 from Penlon
The Prima 465 is designed to withstand the demands of a busy OR.
Important Features: It has a “ventilator with touch-screen control” but still has a very tactile, user-friendly appearance. It is renowned for being incredibly small.
Benefits: It’s a “back-to-basics” device that respects the anesthesiologist’s time. It is dependable, follows instructions, and doesn’t malfunction.
Advantages: It is very simple to maintain and clean. Its compact footprint is suitable in small operating rooms.
Disadvantages: Some of the most sophisticated AI-driven ventilation modes available on the high-end Dräger or GE versions are absent.
How to Buy Anesthesia Machines
If your hospital is planning to get a machine for anesthesia, here are tips to consider:
Evaluate the scope of your clinical work.
Knowing the “who” and “where” of your facility is essential before you make your choice. For a specialist dental surgery room, the equipment made for a high-volume trauma hospital is excessive.
- Patient profiles: Do you primarily treat adults, children, or newborns? Sensitive neonatal modes on certain equipment are vital for smaller patients.
- Complexity of Procedure: Are you doing simple outpatient operations or complex neurosurgeries that take hours? For the second, your clinic needs an advanced ventilation mode (such as SIMV or PRVC).
Give user experience and ergonomics top priority.
Usually, anesthesiologists stay close to this equipment for eight to ten hours during operation. So, the interface should be user-friendly.
- Intuitive Controls: How responsive is the touchscreen? Are the alarm systems easy to deactivate and read? You don’t want to be searching through submenus to change the oxygen flow in an emergency.
- Workspace Design: Does the device have enough shelves for charts and monitors? Are the drawers quiet and smooth? The anesthesiologist’s cognitive load is lessened by a simple workspace.
Assess Lifecycle Expenses and Reliability
You may want to evaluate the “Total Cost of Ownership.
- Maintenance Contracts: Find out whether local service specialists are nearby. How many hours will your operating room be offline while you wait for a part if the equipment breaks down?
- Consumables: Check the price of soda-lime canisters, O₂ cells, and proprietary sensors. Sometimes, a cheaper machine costs more because it needs expensive, brand-specific filters.
The Inspection Checklist
If you are buying a refurbished or pre-owned anesthesia machines, check the following:
Calibration History: Request the service logs. Has it undergone an annual professional calibration?
- Battery Backup: Examine the internal power supply. Make sure that the battery can last at least 30 to 60 minutes if the facility loses power.
- Software Updates: Know this: The safety precautions present in more recent software versions might not be present in older devices.
Involve the Final Users
The most important step is this one. Never buy an anesthetic machine without allowing your anesthesia team to “test drive” it.
Practical Demos: Ask suppliers to visit your establishment with a demonstration unit. Do a mock setup with your CRNA or lead anesthesiologist.
The “Feel” Factor: Find out from the clinicians whether the flow feels seamless. Is it simple to connect the breathing circuit? Do you think you can use this machine with a patient?
Reliability is essential in a high-stakes operating room. Make sure the unit has the necessary FDA, ISO, and CE certifications before deciding. These badges assure you that the device has met the international standard for patient monitoring, pressure control, and safety.
“Never concentrate only on the eye-catching touchscreen interface. Order the manual override features at all times. Make sure that your backup gas delivery and ventilation systems can function under high pressure.”
Future-Proofing on Anesthesia Machines
Nothing is more annoying than spending money on equipment that feels “old” as soon as it is installed. Future-proofing includes software upgradeability and modularity in addition to glossy screens.
Instead, look for machines that enable you to add new ventilation modes or sophisticated monitoring tools through software upgrades.
Do you think this machine can adapt if the care standards change in five years? Consider these:
Likability
Attempting to maintain patient stability while writing down numbers or manually transcribing data. It diverts your attention from the patient.
Your digital ecosystem is modern devices. Go for smooth interaction with your electronic medical records (EMR) or anesthesia information management system (AIMS). You want a computer that exports data automatically? Then get the machine connected to your EMR with ease.
Low-Flow Anesthesia
Low-flow anesthetics are becoming popular, and for good reason. In addition to lowering the quantity of costly anesthetic chemicals released into the atmosphere, it makes the patient’s breathing environment warmer, which may enhance their recuperation.
Read also: Best Surgical Tables in 2026 ( Uses, Features and Benefits
Wrapping Up
High-end anesthetic workstations are unquestionably important in today’s operating rooms. The standard in gas delivery and ventilation management is provided by devices such as the GE Aisys CS2 and the Dräger Perseus A500.
If you combine easy-to-use user interfaces with seamless patient monitoring, these machines reduce the cognitive load during critical procedures.
Medical teams put patient safety first by investing such dependable hardware. Meaning that with these instruments in a surgical suite, it changes the therapeutic experience.
-

 Diagnostic & Hospital Equipments4 months ago
Diagnostic & Hospital Equipments4 months agoWhat Are Medical Devices? Types and Uses
-

 Uncategorized4 months ago
Uncategorized4 months ago6 Best Heatmap Plugins – I Test, Review and Compare
-

 AI in Health care4 months ago
AI in Health care4 months agoRemote Patient Monitoring in Modern Healthcare
-

 AI in Health care2 months ago
AI in Health care2 months agoDigital X-ray vs. Film X-ray: Which is better?
-

 AI in Health care4 months ago
AI in Health care4 months agoAI in Medical Imaging: What is Coming Next
-
 Review and guides3 months ago
Review and guides3 months agoCPAP Machines Buying Guide: The Best Models Doctors Don’t Recommend
-
 Diagnostic & Hospital Equipments1 month ago
Diagnostic & Hospital Equipments1 month agoDEXA Bone Density Scanning: What You Need to Know About Bone Health
-
 Diagnostic & Hospital Equipments1 month ago
Diagnostic & Hospital Equipments1 month agoPET Scan Machines: Understanding the Technology, and Usage


