Diagnostic & Hospital Equipments
How to Clean Medical Devices Properly: Costly Mistakes to Avoid

Cleaning medical devices is not just wiping the surfaces. So, we will share with you how to clean medical devices properly. You must remove the bioburden, avoid cross-contamination, and use disinfection or sterilization effectively. In hospital settings, inadequate cleaning is a major cause of sterilization failure.
Organic matter, such as blood and tissue, can protect microorganisms from disinfectants and the penetration of steam. At that point, not even an autoclave run will render them sterile. For this reason, cleaning always precedes disinfection or sterilization.
To clean medical devices effectively, follow established reprocessing phase. These phases are standard for all SPD areas (Sterile Processing Department) and integrate well-known infection prevention models. There is a reason for each level, and omitting one breaks the chain.
How to Clean Medical Devices Properly
Basically, to clean a medical device, it depends on the device. The universal applied method is the Spaulding Classification. This classification is core to CDC and AAMI recommendations. They fall into the following groups:
Critical Devices
Critical devices contact sterile tissue or the bloodstream. These are surgical instruments, implants, and cardiac catheters. They must be sterilized before you use them. Sterilization helps destroy all forms of microbial life, including bacterial spores.
Steam sterilization (autoclaving) is the best validated process for heat-resistant instruments. Other techniques, like ethylene oxide gas or hydrogen peroxide vapor, are used for heat-sensitive products.
Medical devices must be thoroughly cleaned before sterilization. The remaining bioburden may protect microorganisms from penetrating the steam.
Semi-critical Devices
In cleaning semi-critical devices, you need to understand that there is contact with mucous membranes or non-intact skin. These are endoscopes and respiratory therapy apparatus.
These need to be at least high-level disinfected. High-level disinfectants can be glutaraldehyde, ortho-phthalaldehyde, or hydrogen peroxide-based formulations. Observance contact time should be observed strictly and follow the manufacturer’s instructions.
Non-critical Devices
Noncritical devices touch only the intact skin. These include blood pressure cuffs, stethoscopes, pulse oximeters, and bed rails.
These must be cleaned and then low-level disinfected with agents only approved, e.g., 70% isopropyl alcohol or quaternary ammonium salts.
Proper classification will ensure that the cleaning is commensurate with the risk of infection.
Step 1: Point-of-Use Pre-Treatment in Cleaning Medical Devices
Cleaning starts right after use
They begin to dry. Blood and organic material start drying within moments. Once dried, proteins stick tight to surfaces and can be challenging to remove. However, if removed early, it reduces both cleaning time and the risk of contracting infection.
At the point of care:
- Use a non-reusable cloth to wipe off the gross soil.
- Rinse with water if the device is water-compatible.
- Moisten instruments with enzymatic pretreatment sprays or wet towels.
- Don’t soak in saline, because chloride ions accelerate rusting.
And a technically critical tip: Use cold or lukewarm water for the first rinse. Hot water coagulates proteins such as blood and makes them stick to the surface. Point-of-use care preserves instrument integrity and enhances the success of cleaning downstream.
Step 2: Cleaning (Manual and Mechanical Cleaning)
Chemical and physical cleaning removes organic and inorganic matter. This stage will perhaps determine the success or failure of subsequent disinfection or sterilization.
Manual cleaning
Heat-sensitive or intricate instruments need to be cleaned manually.
The Access Control: T&C has the following features:
- Submersion in a neutral-pH-based enzymatic detergent.
Use low-foaming products to avoid any residues.
- Wash to reduce aerosol production.
- Use appropriate brushes to clean the valves and narrow passages.
Follow the manufacturer’s recommendations. Insufficient dilution can affect the result, and over-dilution will leave residue. In addition, work on the hinges, serrations, and lumen. These places are difficult to clean and are areas that traps bioburden easily.
How to Clean Medical Devices: Mechanical cleaning
With mechanical cleaning, it quickens the cleaning process and is very reliable because it reduces frequent touching. The mechanical cleaning requires washer-disinfectors that operate validated cycles with washing, rinsing, and application of thermal disinfection. Loading is important:
- Hinged instruments should be opened.
- There shouldn’t be any obstacles to the spray arms.
- Attach Lumens to irrigation.
Ultrasonic cleaners remove debris from intricate surfaces through cavitation. They are suitable for precision tools, but they are not a substitute for washer-disinfectors.
Cycle patterns, time, detergent concentration, and temperature must follow the device manufacturer’s instructions.
Step 3: Rinsing and Inspection
Intensive rinsing eliminates detergent residues and detached soil after cleaning.
Final rinse water may be treated, deionized, or sterilized in line with the protocol of your facility. Untreated hard water can cause scale and rust.
Inspection is mandatory.
Make sure that there is no:
- Residual debris on the device
- Corrosion or pitting
- Cracks
- Functional movement
- Lumen integrity
Step 4: Disinfection and Sterilization
The classification determines the technique.
Sterilization for Critical Devices
Valid cycle considerations are required for steam sterilization. Monitoring includes:
- Mechanical indicators (time, temperature, pressure)
- Chemical indicators inside the packages
- Biological indicators based on resistant spores
These indicate that the sterilization process was conducted under the desired conditions.
High-Level Disinfection for Semi-critical Devices
Chemical disinfectants should meet the contact time requirements based on the manufacturer’s instructions. Also, rinse devices after disinfection; use sterile or filtered water to remove chemical residues.
Additional steps for flexible endoscopes include channel flushing and forced-air drying.
Low-Level Disinfection for Non-critical Medical Devices
- Approved disinfectant wipes or alcohol-based solutions are used on surfaces that come in contact with unbroken skin.
- Keep the surface wet for the entire contact time. Drying prematurely decreases microbial kill.
Step 5: Drying and Storing
Microbial growth increases, and packaging weakens by moisture.
Effective drying includes:
- Dry with a lint-free cloth.
- Medical compressed air for lumens
- Complete internal dryness (air cannot be trapped within the lumen)
Clean the storage environment. Safeguard sterile packages from moisture and physical harm.
Poor storage can contaminate devices even if they are sterilized properly.
Water Quality and Detergent
The durability of the instrument is influenced by the hard water. Staining and corrosion from mineral deposits. Reverse osmosis systems are used by many institutions to treat water.
Detergent type is important. Enzymatic detergents degrade protein and fatty deposits. Neutral pH-based formulations help maintain the surface finish of the medical device. The wrong detergent also reduces the life of the device.
Documentation and Quality Assurance
Facilities must document:
- Cleaning cycles
- Sterilization parameters
- Results of biological indicators
- Maintenance of equipment
Quality control ensures reproducible experiments and patient safety.
Guidance documents (e.g., AAMI ST79) exist for many aspects of steam sterilization and sterile processing workflow.
How to Clean Medical Devices at Home
For home-use products, such as nebulizers or glucose monitors:
- Clean immediately after handling.
- Stick to the manufacturer’s instructions.
- Use a mild detergent unless directed otherwise.
- Let it dry completely before you store them.
- Replace parts when weak or damaged.
Never immerse electronic parts unless you are using them at home, and the manufacturer explicitly states this is allowed.
How to Choose the Best Cleaning Solution for Medical Devices
Choose disinfectants that are:
- Registered with the EPA (if appropriate)
- Device material compatible
- Able to kill the most common viruses and bacteria
Common Types:
- Alcohol-based products
- Quaternary ammonium compounds (Quats)
- Hydrogen peroxide towelettes
Make sure to check for compatibility.
Signs a Medical Device is “Cracked” by Overcleaning
Excessive cleaning can damage equipment.
Watch for:
- Cracking plastic
- Faded displays
- Stiff tubing
- Corrosion.
Recommended Cleaning Periods
Related: Why Your Glucose Monitor Is Giving Wrong Reading and What to Buy Instead
- Personal home use: after each use
- Shared family device: each person’s use
- Clinic device: with every patient
Mistakes People Make When Cleaning Medical Devices
Small errors in reprocessing can damage the device, cause sterilization cycle failures, regulatory concerns, and, in more severe instances, patient injury.
Here are mistakes you can’t afford to make.
1. Delay Point-of-Use Cleaning
Allowing blood and body fluids to harden on instruments is one of the common mistakes people make when cleaning medical devices.
When organic matter dries, proteins harden and strongly bond to surfaces. These factors makes cleaning such items more difficult and increases the possibility of having some debris after washing.
Also, keep the devices moist and clean right after using them. The mistake many lab technologists make is waiting waiting until the end of a procedure list or shift.
2. Using Hot Water for the Initial Rinse
Warm or hot water in the warm-up stages of cleaning is a cooking mistake.
Heat causes the protein to coagulate. Hot water makes the blood “cook” on the bit of the instrument. Once it’s coagulated, it’s more painful to take it off, and you have to use some elbow grease, which might harm the device.
The first rinse should always be under cool or warm water unless the manufacturer’s instructions state otherwise.
3. Using abrasive tools or chemicals
One big mistake is scrubbing delicate instruments with abrasive brushes, steel wool, or chemicals, including bleach.
Don’t use abrasive cleaning materials or harsh chemicals on your instruments, such as bleach, which can lead to pitting and erosion of delicate instruments.
Bleach can also damage stainless steel because of its chloride content. Micropitting results in the formation of micro-crevices that could harbor bacteria. When pitting begins, instruments become more difficult to clean and may need to be replaced sooner.
Only use the detergents and disinfectants approved by the manufacturer. Cleaning agents should be suitable for the material of the device.
4. Overloading of washer-disinfectors
Consistent results are better with mechanical washing but only if you load them right. Do not overfill the trays or stack the instruments, as this will prevent the water and detergent from reaching them. Spray arms blocked. Stop them from working effectively.
Closed-hinged device cannot be cleaned inside because the internal surfaces are not accessible. Loading too heavily may not remove particles completely.
5. Skipping Inspection Before Disinfection or Sterilization
Sometimes, people in charge do the job haphazardly. This is a terrible mistake. Once clean, examine each device for the following:
- Residual debris
- Corrosion
- Cracks
- Functionality
If particle is still present, take it back to the cleaning stage. Going on to sterilization with debris will not sterile it properly. Do not replace cleaning for sterilization. Inspection is the final checkpoint before a device moves forward in the reprocessing chain.
FAQs About How to Clean Medical Devices
1. How often should we clean medical devices?
Ideally, you should clean Medical devices such as blood pressure cuffs after each use, particularly when they have contact with skin or body fluids. Devices shared with more than one person must be sterilized before using on another person.
In healthcare environments, how often you clean will vary by device classification (i.e., the classification is critical, semi-critical, or non-critical). Don’t wait until the device “looks dirty.” You can’t see microorganisms.
2. Is 70% alcohol sufficient to clean medical equipment?
Seventy percent isopropyl alcohol can be used on many non-critical items, such as thermometers and pulse oximeters. But it can be unsafe for certain materials and cannot replace high-level disinfection or sterilization when the latter is necessary. Always use the manufacturer’s cleaning recommendations.
3. What is the difference between cleaning and disinfecting?
Cleaning is the removal of dirt and organic matter from an instrument. Disinfecting kills many harmful microorganisms, but not all spores, necessarily. Sterilization kills all microbial life. Cleaning should always precede disinfection or sterilization.
4. Can improper cleaning damage medical devices?
Yes. Strong chemicals, too much moisture, or abrasive materials can damage sensors, plastics, and electronics. This could lead to device de-calibration and reduced device life expectancy or failure. Always use approved cleaning agents and do not soak electronic parts.
5. How long should I leave the disinfectant on the device?
The disinfectant should stay on the surface during the entire contact time from the product label. This can be from 30 seconds to minutes. Drying too fast makes the disinfection less effective.
Conclusion On How to Clean Medical Devices
To clean medical devices properly, it requires validated steps such as point-of-use pre-treatment, cleaning, rinsing and inspection, disinfection or sterilization according to risk classification, drying, and storage.
However, you must follow each stage appropriately. If you miss any step, it may attract bacteria that can cause infection in users.
Now you know how to clean medical devices properly. Hope it was helpful. Kindly share on your pages. For your comments and suggestions, use the comment section.
Diagnostic & Hospital Equipments
Top 5 Anesthesia Machines for Hospitals That Deliver Performance
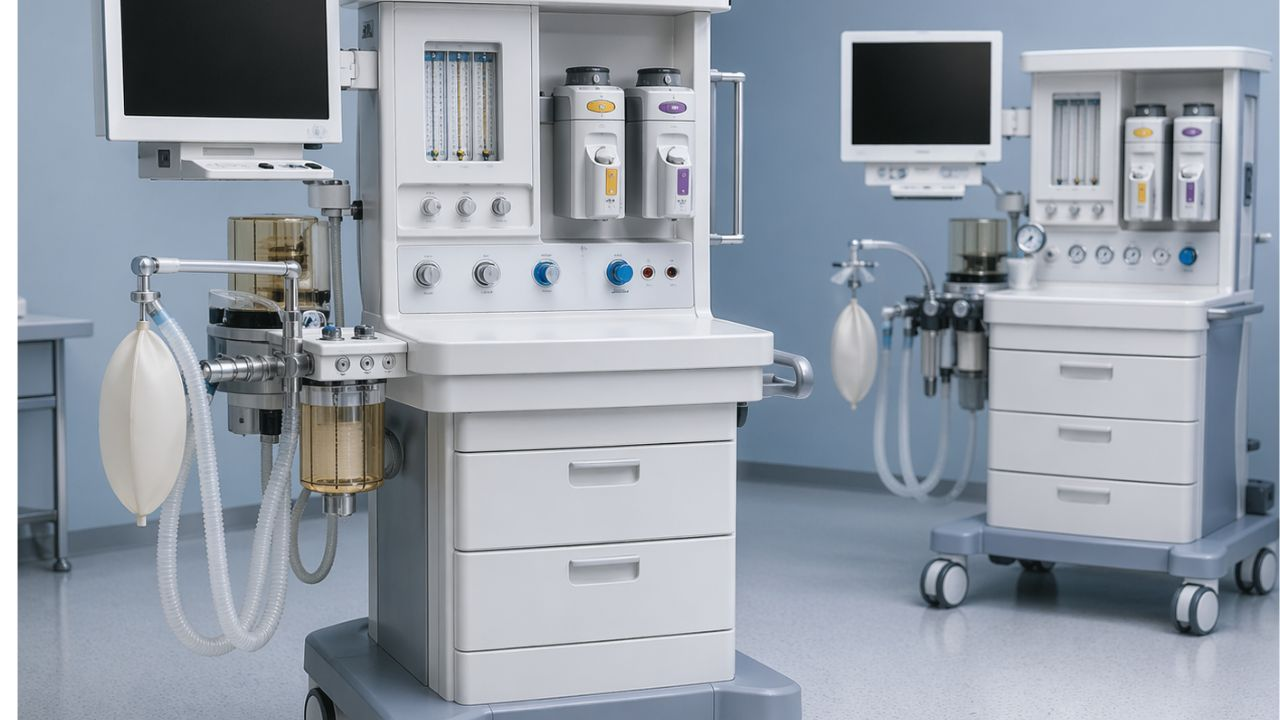
In a busy operating room, the line between a simple surgery and a serious emergency depends on the reliability of equipment and surgeons’ expertise. When a surgeon starts operating, they need tools that will make their job easy, which is exactly what you get with today’s anesthesia machines.
For the anesthesiologist, this machine is key. It’s the link between the patient being awake and them undergoing a pain-free, life-saving procedure. It lets them keep a close eye on the patient’s body functions while the surgeons do their thing.
Every successful surgery is backed by the confidence these machines give. Nowadays, companies make anesthesia machines with advanced breathing and monitoring features.
What is an Anesthesia Machine used for?
Basically, an anesthesia machine mixes oxygen and anesthetic gases to keep the patient asleep and doesn’t feel any pain. It also acts like a breathing machine.
The machine has fancy screens that show things like heart rate, blood pressure, etc. For the anesthesiologist, these numbers are like a way to talk to the patient’s body. If things change, the doctor tweaks the controls. It’s this continuous back-and-forth that keeps the patient in a safe, controlled state of unconsciousness.
What are the 4 types of Anesthesia?
When it comes to surgery and other medical procedures, four main types of anesthesia can be used. They are:
1. General Anesthesia
This type of anesthesia puts a patient into a controlled sleep. The anesthesiologist gives the patient strong medications that stop pain signals from getting to the brain. When the person wakes up, they won’t remember anything about the surgery.
2. Regional Anesthesia
The regional anesthesia numbs a larger part of your body, like the arm, the leg, or the whole lower half. They inject medication near a group of nerves to create a temporary “no feeling” zone for pain. However, an epidural, for example, is injected into the spinal canal and can also be used for childbirth.
With this, the patient can stay awake and chat with the doctor, but your lower body won’t feel a thing during the procedure.
3. Monitored Anesthesia
Often referred to as “twilight sedation,” the monitored anesthesia puts you in a sort of dream-like state. You’re not completely unconscious but relaxed and won’t notice any surgery taking place on your body.
This is mostly used for quick procedures. It’s a nice middle ground between being fully awake and completely asleep.
4. Local Anesthesia
The local anesthesia is the most basic type, used for small surgeries like cuts or biopsies. A numbing liquid (Betadine) is applied to the skin, in the mouth, or injected into the tissue. Local anesthesia is good for procedures that don’t take too long, usually under two hours, such as dental work or taking small tissue samples.
While it’s usually very safe, some people may have reactions like allergies or feel some tingling, burning, or swelling.
Top Anesthesia Machines
Selecting the most suitable anesthesia machine depends on factors such as the hospital’s budget, the clinical requirements, and the preferences of the anesthesiologists. Here are some of the top options available.
GE Healthcare’s Aisys CS2
The Aisys CS2 is a modern version of long-standing operating room machines. Its digital features ensure precise gas delivery and smooth integration with electronic health records.
- Advantage: It has a clean interface and enough ventilation. Also, the parts are easy to get.
- Disadvantage: Expensive due to the high-tech digital features.
- Popular because it’s familiar to those who trained on Ohmeda machines.
Dräger Anesthesia Machines
Dräger’s Perseus A500 is a sophisticated anesthesia machine known for its sleek design and automation. It adapts well to different patient sizes and includes automatic lung recruitment operations.
- Benefit: Saves space
- Advantages: Has a beautiful custom screen layout. Doesn’t make noise and does much of the work for you.
- Disadvantage: Requires software training.
- Popular due to the automation and advanced ventilation options.
Mindray: A9
Mindray used to be considered the “budget” alternative, but the A9 has transformed that notion. It’s not as expensive as the Aisys CS2; however, it serves well.
The benefit is that it serves as a “workhorse,” dependable, and user-friendly.
Key features include a large, easy-to-read touchscreen and an integrated “High-Flow Nasal Cannula” mode.
Advantages: Offers excellent value for the price. You get high-end features (such as improved ventilation).
Disadvantages: The build quality is acceptable, but not durable like previous GE or Dräger units. Some clinicians still need to familiarize themselves with the UI.
Why hospitals like it: For hospitals that desire high-end technology, it is still affordable.
IntelliSave AX700 from Philips
It makes perfect sense that Philips has an anesthesia machine that communicates easily with their monitor systems. The company is famous as a reliable brand for patient monitoring.
- Benefits: If your hospital is already a “Philips shop,” this makes more sense. The flow of data is incomparable.
- Key Features: It’s incredible how it integrates with Philips patient monitors. It lessens the “alarm fatigue” that so many medical professionals experience.
- The Advantages: Unified. Instead of feeling like a machine and a monitor pasted together, it works as a single, coherent system.
- Disadvantages: It is nearly overly integrated. The device may feel a little limiting if you don’t like the Philips ecosystem.
- Popular for: The data storage is the main reason people go for it. This device is perfect for anesthesiologists who enjoy having all their patients’ vital signs and breathing data in a synchronized stream.
Prima 465 from Penlon
The Prima 465 is designed to withstand the demands of a busy OR.
Important Features: It has a “ventilator with touch-screen control” but still has a very tactile, user-friendly appearance. It is renowned for being incredibly small.
Benefits: It’s a “back-to-basics” device that respects the anesthesiologist’s time. It is dependable, follows instructions, and doesn’t malfunction.
Advantages: It is very simple to maintain and clean. Its compact footprint is suitable in small operating rooms.
Disadvantages: Some of the most sophisticated AI-driven ventilation modes available on the high-end Dräger or GE versions are absent.
How to Buy Anesthesia Machines
If your hospital is planning to get a machine for anesthesia, here are tips to consider:
Evaluate the scope of your clinical work.
Knowing the “who” and “where” of your facility is essential before you make your choice. For a specialist dental surgery room, the equipment made for a high-volume trauma hospital is excessive.
- Patient profiles: Do you primarily treat adults, children, or newborns? Sensitive neonatal modes on certain equipment are vital for smaller patients.
- Complexity of Procedure: Are you doing simple outpatient operations or complex neurosurgeries that take hours? For the second, your clinic needs an advanced ventilation mode (such as SIMV or PRVC).
Give user experience and ergonomics top priority.
Usually, anesthesiologists stay close to this equipment for eight to ten hours during operation. So, the interface should be user-friendly.
- Intuitive Controls: How responsive is the touchscreen? Are the alarm systems easy to deactivate and read? You don’t want to be searching through submenus to change the oxygen flow in an emergency.
- Workspace Design: Does the device have enough shelves for charts and monitors? Are the drawers quiet and smooth? The anesthesiologist’s cognitive load is lessened by a simple workspace.
Assess Lifecycle Expenses and Reliability
You may want to evaluate the “Total Cost of Ownership.
- Maintenance Contracts: Find out whether local service specialists are nearby. How many hours will your operating room be offline while you wait for a part if the equipment breaks down?
- Consumables: Check the price of soda-lime canisters, O₂ cells, and proprietary sensors. Sometimes, a cheaper machine costs more because it needs expensive, brand-specific filters.
The Inspection Checklist
If you are buying a refurbished or pre-owned anesthesia machines, check the following:
Calibration History: Request the service logs. Has it undergone an annual professional calibration?
- Battery Backup: Examine the internal power supply. Make sure that the battery can last at least 30 to 60 minutes if the facility loses power.
- Software Updates: Know this: The safety precautions present in more recent software versions might not be present in older devices.
Involve the Final Users
The most important step is this one. Never buy an anesthetic machine without allowing your anesthesia team to “test drive” it.
Practical Demos: Ask suppliers to visit your establishment with a demonstration unit. Do a mock setup with your CRNA or lead anesthesiologist.
The “Feel” Factor: Find out from the clinicians whether the flow feels seamless. Is it simple to connect the breathing circuit? Do you think you can use this machine with a patient?
Reliability is essential in a high-stakes operating room. Make sure the unit has the necessary FDA, ISO, and CE certifications before deciding. These badges assure you that the device has met the international standard for patient monitoring, pressure control, and safety.
“Never concentrate only on the eye-catching touchscreen interface. Order the manual override features at all times. Make sure that your backup gas delivery and ventilation systems can function under high pressure.”
Future-Proofing on Anesthesia Machines
Nothing is more annoying than spending money on equipment that feels “old” as soon as it is installed. Future-proofing includes software upgradeability and modularity in addition to glossy screens.
Instead, look for machines that enable you to add new ventilation modes or sophisticated monitoring tools through software upgrades.
Do you think this machine can adapt if the care standards change in five years? Consider these:
Likability
Attempting to maintain patient stability while writing down numbers or manually transcribing data. It diverts your attention from the patient.
Your digital ecosystem is modern devices. Go for smooth interaction with your electronic medical records (EMR) or anesthesia information management system (AIMS). You want a computer that exports data automatically? Then get the machine connected to your EMR with ease.
Low-Flow Anesthesia
Low-flow anesthetics are becoming popular, and for good reason. In addition to lowering the quantity of costly anesthetic chemicals released into the atmosphere, it makes the patient’s breathing environment warmer, which may enhance their recuperation.
Read also: Best Surgical Tables in 2026 ( Uses, Features and Benefits
Wrapping Up
High-end anesthetic workstations are unquestionably important in today’s operating rooms. The standard in gas delivery and ventilation management is provided by devices such as the GE Aisys CS2 and the Dräger Perseus A500.
If you combine easy-to-use user interfaces with seamless patient monitoring, these machines reduce the cognitive load during critical procedures.
Medical teams put patient safety first by investing such dependable hardware. Meaning that with these instruments in a surgical suite, it changes the therapeutic experience.
Diagnostic & Hospital Equipments
Best Surgical Tables in 2026 ( Uses, Features and Benefits

A surgical table is an advanced medical device that patients lie on during surgery. Robotic assistance, real-time imaging, and data-driven ergonomic design, however, has made it difficult to select the appropriate surgical tables.
Hospitals don’t buy medical equipment’s because of marketing claims from social media influencers; they go for the benefit it offers, capacity, and sometimes availability. As the need for surgical operations is increasing, the best healthcare facilities can do is to get devices that are clinically tested and patient-friendly.
What is a Surgical Table?
An operating table, also called a surgical table, is not a regular flat-surfaced table, it functions as an adaptable work platform, that requires stability when performing surgical operations.
It ensures proper patient positioning and allow surgeons to move freely while carrying out a surgery. These tables have modular designs and movable parts that enable precise adjustments. This includes changes in height, side-to-side tilt, and Trendelenburg or reverse Trendelenburg positions for different types of surgeries.
Modern tables are classified according to their clinical use, such as radiolucent tables made especially to work with X-rays and C-arm imaging, orthopedic, neurological, or general surgery. Pressure-relieving cushioning to stop skin deterioration and a variety of attachments, such as arm boards, stirrups, and headrests.
Many are driven by electro-hydraulic systems, which allow the surgical team to make seamless adjustments using a remote control.
What Defines a “Best-in-Class” Table?
We must know the three foundations of surgical technology before we discuss the best models. They are:
- AI-Driven: To reduce the danger of pressure ulcers and nerve damage during lengthy procedures, modern tables now use weight-distribution sensors to recommend the ideal Trendelenburg angle.
- Total Radiolucency: As a hybrid becomes more common, 360-degree carbon-fiber tops are used because they allow intraoperative fluoroscopy and CT without moving the patient.
- Robotic Syncing: To preserve the balance of the surgical field, some facilities integrate robotic platforms (such as Da Vinci or Hugo) into their operating tables.
Surgical Tables and their Uses
Maquet (Getinge)
Maquet, a Getinge Group brand, is always at the top of the list when it comes to the best surgical tables available on the market. With a history spanning more than 180 years, Maquet is now under the Getinge umbrella. From the mobile Maquet Meera to the modular Maquet Magnus, their surgical tables can handle both simple outpatient operations and multidisciplinary surgeries.
Uses:
General Surgery: Offers the steady support and comfort positioning required for procedures on the abdomen, gastrointestinal tract and other soft tissue areas.
Orthopedics and Traumatology: Maquet tables provide the precise traction and positioning for hip replacements, fracture fixations, and spinal alignments through their customized extensions.
Cardiovascular and Hybrid: These tables deliver minimally invasive heart and vascular procedures and can be integrated with advanced imaging systems (such as C-arms).
Neurosurgery: For delicate cranial procedures, it is compatible with skull clamps and specialty headrests.
Bariatric surgery: Helps to sustain high weight capacities.
Features of Maquet (Getinge) Tables
- Modular tabletop system
- Extreme Articulation and Positioning
- Superior Radiolucency
- Advanced Ergonomics and Intuitive Controls
- Auto-Drive)
Benefits:
Patient-friendly
The table’s ergonomic structure has specialized pressure-distributing pads (SFC padding) that reduce nerve injuries during extended procedures. Secure locking mechanisms maintain patient stability, even when the table is tilted to extreme positions.
Workflow Efficiency
Modular “transporter” components enable patients to be positioned outside the operating room before being moved directly onto the table base. This streamlines room transitions, cutting down turnover time and supporting a higher volume of surgeries each day.
Future-Proofing the OR
Maquet tables can integrate seamlessly with advanced 3D imaging technologies. Also, they can adapt as medical innovations progress.
Maquet Models to Consider
- Maquet Magnus
- Maquet Meera
- Maquet Alphamaquet
Skytron
Because of its user-friendly concept, Skytron is a favorite among surgeons and nurses. In terms of total-room maneuverability, the Skytron 3600 and 3500 Series are the top choices.
But this consistent reputation? Is it a strong brand presence, or is there a difference in how these tables function?
Unlike some manufacturers that concentrate on a single specialty, Skytron creates adaptable tables to serve multi-purpose solutions across hospital settings.
Uses for Skytron Surgical Tables
You’ll find them used across several medical specialties, such as:
- General Surgery: Handles routine appendectomies to complex abdominal procedures.
- Bariatric Surgery: Skytron has high weight-bearing capabilities.
- Orthopedics: Their tables provide the necessary traction and severe angles for knee and hip replacements.
- Cardiovascular & Neurology: They are ideal for operations that requires C-arm access because of their compatibility with medical imaging devices.
- Urology and Gynecology: Offer smooth, and accurate adjustments for tilting and lithotomy positions, enhancing procedural precision.
Features
- 270° to 360° Tabletop Rotation
- Industry-Leading Weight Capacity (Many models can support up to 1,000 lbs of lift and 800 lbs)
- Massive Top Slide
- Low-Profile Base
Benefits:
Patient Safety
Has an auto-beach chair with positioning and locking mechanisms that reduce the chance of the patient’s movement or slipping during procedures. These tables maintain steadiness, even when tilted too high.
Comfort
During lengthy microsurgeries when the table is lowered, or when working at elevated levels, it reduces back strain on tall surgeons.
Durable
Constructed from high-grade materials, these tables tolerate frequent exposure to chemicals and the constant use in high-volume trauma environments.
Efficient
Since a single Skytron table can replace three specialized units, hospitals benefit from reduced equipment needs, lower storage demands, and cheap costs to manage multiple devices.
Steris
While Skytron emphasizes mobility, Steris focuses on smart functionality. The Steris 5085 and 4085 models are the most dependable, and they can be integrated with hospital electronic medical record (EMR) systems.
These tables are efficient, whether in a small outpatient surgery center or a large, high-volume Level 1 trauma facility.
Uses for STERIS Surgical Tables:
General and Bariatric Surgery
Many models can carry patients weighing 1,000 lbs. These strengths are essential for bariatric surgeries, where safety and secure positioning are paramount.
Orthopedic and Spinal Surgeries
Precision in patient positioning is essential during orthopedic and spine operations. STERIS tables are compatible with a variety of specialized attachments that enable accurate limb alignment or facilitate prone positioning, such as tucking.
Their seamless integration with carbon fiber components also gives surgeons unobstructed access to the skeletal area, making these tables a preferred choice in complex bone and spine cases.
Advanced C-Arm Imaging
With the growing use of minimally invasive techniques, high-quality imaging has become important. STERIS tables have extensive radiolucent sections that allow clear X-ray imaging and efficient C-arm use. This design removes the need to reposition patients or deal with metal interference.
Features:
- Auto-Limit Sensors
- Exceptional Articulation.
- Intuitive Hand Controls
- Radiolucent Tabletops
- Self-Leveling Floor Locks
- Modular Design
The Benefits:
Lowers the Chance of Falls
Intraoperative falls and pressure injuries are less likely to occur when there is stability. High-quality pressure-reduction pads are used in conjunction with STERIS tables to distribute a patient’s weight and prevent bedsores, which can develop during extended, multi-hour marathons.
Enhanced Staff Ergonomics
The tallest surgeons and the lowest technicians may operate in a position that doesn’t damage their backs due to their height adjustments.
Berchtold Operon (Stryker)
The Berchtold Operon (D-Series), now part of the Stryker ecosystem, has established itself as one of the leading options for bariatric and orthopedic trauma procedures. German engineering and American innovation are combined in models such as the D850, D820, and D760. These are multipurpose surgical tables with sliding tops that may be used for nearly any operation.
Uses:
- General Operation: Equipped with specific accessories, it can be used for different types of surgeries.
- Orthopedics: Suitable for hip replacement.
- Cardiovascular & Urology: Its radiolucent design allows uninterrupted C-arm imaging, which is why it is ideal for image-guided interventions.
- Bariatric Surgery: With a high weight limit, it offers secure and stable support for patients needing additional capacity.
- Neurosurgery: During microsurgery, the Operon’s stability guarantees that delicate head-frame attachments stay stable.
Features:
- Massive Weight Capacity: The Operon D860 can support weights up to 1,250 lbs in a level position and 1,000 lbs through a full range of motion.
- Carbon Fiber Integration
- Sliding Top
- Ergonomic Hand Control
- Superior Articulation
The Benefits:
Sturdy
Even during high-torque orthopedic surgery, the table won’t move because of the floor-locking system. In addition, the pressure-relieving pads lessen the chance of “bedsores” during extended table time.
Dependable
This table offers the foundation required for heavy-duty surgical workflows for facilities that are seeing a rise in bariatric patients or those who have invested in the Stryker iSuite (the integrated digital operating room).
Mizuho OSI
When it comes to patient positioning, especially for orthopedic and spine surgeries, Mizuho OSI is still the undisputed choice. Their tables address the physical constraints that surgeons encounter, whether they are used for sophisticated imaging, orthopedic trauma, or spinal surgery. The ProAxis and Trios systems are top models.
Uses and Clinical Applications:
Spine Surgery: For spine surgeries, the Jackson Table is the industry standard. It enables advanced prone placement, lowers intra-abdominal pressure and enhances hemodynamics.
Orthopedic Trauma: Their platforms can handle the traction needed for tibia and femur fractures. It gives surgeons the stability they need to achieve ideal alignment.
Comprehensive Imaging: In settings where intraoperative C-arm imaging is required, these tables are essential due to their open frame design.
Features:
- Software-Controlled Positioning: The ProAxis table features motorized joints that resemble natural human movement.
- Radiolucent Dual-Column Structure: The table’s design creates unrestricted 360-degree C-arm rotation around the spine or limbs.
Benefits:
Improved Imaging Precision: Since the table does not interfere with X-rays, clearer images can often be obtained using lower radiation levels, minimizing exposure for both the patient and the surgical team.
Mizuho OSI tables function as essential surgical tools, not just support surfaces. By optimizing spinal alignment and reducing pressure on the vena cava, they help lower the risk of post-surgical complications and pressure injuries during extended procedures.
Read also: Robotic Surgery Systems: Scope, Design, and Implications
Wrapping Up: Which are the best surgical tables in 2026?
To make your choice, select a table specific to the type of surgery your facility performs often. Also, consider the cost setup.
Buy Maquet if your hospital values high-end design and adaptability.
Consider Skytron if speed and maneuverability are what define your operation room.
Steris wins if data integration and safety are the objectives.
Berchtold (Stryker) is for heavy-duty bariatrics and robotic support.
In addition, Mizuho OSI is still the best for difficult spine and orthopedics.
AI in Healthcare
Robotic Surgery Systems: Scope, Design, and Implications

The phrase “robotic surgery” refers to a broad category of surgical platforms that help to facilitate, enhance, or automate tasks human surgeons perform. These platforms include teleoperating systems (controlled by a surgeon), telerobotic systems, and autonomous action (robotic surgery systems).
Some hospitals now center on robotic-assisted surgery. However, recent analysis highlights that questions are yet unanswered: What are the differences in clinical results between surgery performed with robotic assistance and surgery performed traditionally?
What are Robotic Surgery Systems?
With AI, tasks are performed faster, and the healthcare sector is not missing out on this automation. Machines now assist surgeons during operations. The robotic surgery system operates in this manner.
A mechanical arm, fitted with tiny tools, does the cutting and stitching. The doctor watches on a monitor and controls the robot with his/her hands. Basically, this setup provides more precision than hands alone. However, not every hospital uses these systems. Surgeons still make all key decisions.
One piece makes up part of what you see. Another section works behind that one. Then there is a third element that sits separately, but it connects closely to both.
A tiny lens brings sharp images into view during operations. This tool shapes how doctors see inside the body. The surgeon controls each tool. Every motion of the camera follows their hands. This is where precision begins.
With a robotic setup, surgeons can get accurate, smooth movement, and stronger command throughout the surgical operation. Through small cuts in the skin (minimally invasive), robotic surgery moves into the body. This method slips past thick layers of tissue gently.
There are little scars after the operation. In addition, it heals faster. Pain levels drop during recovery thanks to less damage inside. The risk of infection lowers because the openings are smaller. Also, the organs around the surgical area don’t get affected. More importantly, the probability of getting an infection after surgery is slim.
What are the Types of Robotic Surgery?
These machines assist urologists in treating prostate, kidney, and bladder issues. Also, gynecological use of this system involves removing the uterus or fibroid tissue. Even common operations such as fixing hernias or taking out gallbladders benefit from robotic surgery. Interestingly, patients don’t lose much blood during the surgery. To add, complications after surgery are rare, unlike traditional surgery.
Robotic Surgery Stystems By Specialty
Urologic Surgery
Surgeons turn to radical prostatectomy when treating prostate cancer. With robotic help, they take out the prostate but move carefully around nearby nerves. This care helps men keep control over urination after surgery. Sexual function stands a better chance, too.
With partial and radical nephrectomy, a robotic system allows careful removal of diseased parts and still protects working tissue. When treating cancer of the kidney, urologists rely on accuracy found through machine-assisted techniques.
Bladder surgery might take out just a section or the entire organ when dealing with cancer. This kind of operation usually leads to careful rebuilding that demands precision. Sometimes, what comes after depends on how much tissue is affected.
Gynecologic Surgery
- Hysterectomy: Surgical removal of the uterus, are used to treat conditions such as severe bleeding, endometriosis, or cancer. With robotic assistance, creates greater precision in tight anatomical areas.
- Myomectomy: Selective excision of uterine fibroids helps preserve the uterus. It involves smaller incisions compared to traditional open surgery.
- Oophorectomy or Ovarian Cystectomy: The removal of one or both ovaries or ovarian cysts, are used in the treatment of endometriosis or ovarian growths.
Gastrointestinal Surgery
- Cholecystectomy: The gallbladder is removed with robotic assistance, also enables a minimally invasive approach.
- Hernia Repair: Robotic technology have superior visualization, provide accurate mesh placement for both simple and complex abdominal wall hernias.
- Colectomy or Bowel Resection: Portions of the colon can be removed with enhanced precision, and the robotic system supports more controlled reconstruction of the intestinal tract.
Cardiothoracic Surgery
- Mitral Valve Repair: Heart valve repairs are performed through small incisions with robotic tools to prevent the need for an open-chest surgery.
- Cardiac Tissue Ablation: Abnormal heart tissue that causes arrhythmias is targeted and treated with robotic precision.
- Lung Resection and Tumor Removal: Pulmonary tumors or nodules are excised using robotic techniques that improve access to confined areas within the chest.
Head and Neck Surgery
Transoral Robotic Surgery (TORS): Tumors located in the throat, base of the tongue, or tonsils may need external cuts.
Orthopedic Surgery
Joint Replacement (Knee and Hip): Robotic-arm systems such as Mako use personalized 3D imaging to get accurate bone preparation, optimize soft tissue balance, and enhance implant positioning.
What are the 5 Commonly used Robotic Devices?
The top 5 robotic devices seen in many industries, such as manufacturing and medical, include articulated robots (assembly and welding robots), autonomous mobile robots (AMRs) (transportation robots), SCARA robots (fast pick-and-place robots), cobots (robots working alongside humans), and robotic surgical systems (precision surgery robots). Get the details below:
1. Articulated Robot (Industrial Robotic Arm)
This is the most common industrial robotic device. It has 3 to 6 rotating axes that resemble the human arm. Often used for welding, painting, material handling, and machine tending in automotive and manufacturing industries.
2. Autonomous Mobile Robots (AMRs) & AGVs
Robots such as autonomous mobile robots (AMRs) and automated guided vehicles (AGVs) use sensors, cameras & GPS to move parts or finished goods. They are used in warehouses, factories and hospitals. Amazon warehouse robots and the TUG are two popular examples.
3. SCARA Robots
Highly accurate & speedy robots used for precise vertical assembly movements. SCARA robots (as they use 4 axes) are used widely in the electronics industry as well as the car manufacturing industry for tasks including component insertion, packing & assembly.
4. Collaborative Robots (cobots)
Unlike industrial robots, cobots work alongside workers in a factory. They can be quickly programmed for different uses and include tasks such as kitting, machine tending, and packing.
5. Robotic Surgical Systems (medical robots)
These systems are designed for less invasive surgery and allow surgeons to perform complex procedures using robotic arms that has better control and in 3D capacity. For instance, the da Vinci Surgical System, orthopedic robots (e.g., Mako) and robots for sterilization purposes (e.g., Xenex).
The Top Robotic Surgery Systems
Intuitive Surgical: da Vinci Systems (Xi, X, SP, 5)
The industry standard for soft-tissue surgery, for urology, gynecology, and general surgery uses the da Vinci robotic systems. It features high-definition 3D imaging, wristed instruments (EndoWrist), and the new da Vinci 5, that have a force feedback and advanced imaging.
Specialty Platforms: Ion (endoluminal robotic bronchoscopy for lung biopsy).
Stryker: Mako SmartRobotics
Focus: Orthopedic joint replacement (knee and hip).
Details: It uses pre-operative CT scans to create a 3D model, allows surgeons to customize implants and guide robotic arms for precise bone cuts.
Medtronic: Hugo RAS System
It’s for soft-tissue procedures: Medtronic has a modular, open-console design that enables hospitals to use independent robotic arms. It enhances flexibility and affordability.
Specialty Platforms: Mazor (robotic guidance for spine surgery).
CMR Surgical: Versius
Focus: Minimally invasive, versatile surgery.
It’s portable, and designed to fit into existing surgical workflows easily. It is increasingly used in Europe, Australia and India for various laparoscopy procedures.
Asensus Surgical: Senhance System
- Focus: Laparoscopic digital surgery.
- Details: Emphasizes haptic feedback (touch sensation) and eye-tracking camera control, with a high precision.
Globus Medical: ExcelsiusGPS
- Focus: Spine and cranial surgery.
- Details: Provides real-time imaging and robotics-guided precision for spinal fusion and other neurosurgical process.
Zimmer Biomet: ROSA Robotics System
- Focus: Orthopedic surgery.
- Details: Specialized in robot-assisted knee and hip replacements with advanced data analytics for precise positioning.
- Focus: Robotic bronchoscopy.
- Details: Used for early-stage lung cancer diagnosis.
Robotic Surgery Systems’ Growing Effect on Modern Healthcare
Because of smaller incisions used during robotic-assisted surgery, the patient will experience fewer blood losses (an average of 50.5% decrease in loss of blood), a reduced need for transfusions, a shortened recuperation period, and small instances of postoperative infections.
Better control for the surgeon: Robotic systems enable the use of 3D and visualization, which offer a clear and high-resolution view of the surgical site. The robotic arms offer greater dexterity and tremble cancellation and enable the performance of tasks far greater than those performed by human hands.
Growth of new specialties using this technology: While the technology was first widely implemented for prostatectomies within urology, other specialties have adopted it for:
- Gynecology for hysterectomies and endometriosis surgery
- General surgery for hernia repairs, gallbladders, and bariatric surgery procedures
- Orthopedics for joint replacements
- Cardiothoracic surgery for heart valve repair procedures.
Robotic-Assisted Surgery’s System Improvement
Use of AI and Modern Technology
Robotic surgery is getting popular by the day, as leading surgical platforms now use artificial intelligence (AI) to improve decision-making, analytics, and the possibility of personalized medicine. Haptic technology has also become a growing implementation in robotic systems, as it allows surgeons to feel tissue resistance.
Benefits and Challenges of Robotic Surgery
The advantages of robotic surgery include better accuracy, less blood loss, a lower infection rate, and quicker recovery for the patients. Improved visualization and comfortable ergonomics benefit the surgical teams.
Cost, the difficult learning curve for surgeons, and the possibility of technical problems and an increase in operating time are the main disadvantages.
Advantages for the Patients
Increased Speed of Recovery & Less Pain: Patients usually spend less time in the hospital and experience less pain and have a more rapid return to normal life than is typical with conventional surgery.
Decreased Complications: With smaller incisions, there is less risk of infection and a decreased rate of blood loss and clotting.
Increased Accuracy: The ability for the system to make high-precision movements necessary in complicated, meticulous surgery like that done in urology, gynecology, and cardiology.
Improved results in difficult cases: For instance, in robotic prostatectomies and colorectal surgery.
Advantages for the medical team (surgeons and staff)
The 3-D, high-definition, and magnified view available through the system provides the surgeon with the best view possible of the operative field.
The dexterity of the robotic arms is superior to the range of motion and filter for tremors possible with conventional laparoscopy.
The surgeon’s access to improved ergonomics through the seated console position reduces fatigue in the neck, back, and shoulders.
Problems Patients Face
- Cost: Costs can be higher than that of traditional procedures. So, hospital will charge more. Although, it is quicker.
- Possibility of failure: There are risks that an instrument or the robot will malfunction, and that will require it is converted to open surgery.
- Not Suitable for All: Robotic surgery isn’t appropriate for all patients. Discuss with our doctor before using one.
Problems the Medical Team Faces
- Learning Curve: Large amounts of training and simulation time are needed to master the robot system.
- Expensive Investment & Maintenance: Most well-funded hospitals can only afford the cost of the initial acquisition of the robots, including their maintenance.
- No haptic feedback: Surgeons can no longer ‘feel’ with their hands; all surgical feedback must be taken from the camera system.
- Longer setup time: The setup time of the robotic system may increase more time.
Read also: AI in Diagnostic Imaging: What Hospitals Should Know Before Adopting It
Wrapping Up
A robotic surgery system is identified as a surgical robot for minimally invasive surgery. There are two categories: independent robotic surgery systems, in which the entire surgical process is carried out robotically, and assisted laparoscopic surgery systems, where robotic-assisted surgery is used in conjunction with laparoscopy for specific aspects of the procedure.
However, hospital that want to set this should consider the need, capital and and potential return. The best solution must be viewed with a long-term perspective, considering both the investment and benefits.
The questions that addresses robotic surgery systems are: Will the clinical benefits make it a worthwhile investment for a hospital to improve the quality of its service, attract cutting-edge surgeons, and market itself to a wider customer base? and Will the anticipated returns excite an investor with a higher capacity to invest?
We consider investment return based on clinical benefits, effects on the patient, and learning. So, the factors that support or affect the hospital’s decision depend on the hospital’s mission, investment model, and age of patients.
-

 Uncategorized4 months ago
Uncategorized4 months ago6 Best Heatmap Plugins – I Test, Review and Compare
-

 AI in Health care3 months ago
AI in Health care3 months agoRemote Patient Monitoring in Modern Healthcare
-

 Diagnostic & Hospital Equipments4 months ago
Diagnostic & Hospital Equipments4 months agoWhat Are Medical Devices? Types and Uses
-
 Review and guides3 months ago
Review and guides3 months agoCPAP Machines Buying Guide: The Best Models Doctors Don’t Recommend
-

 AI in Health care3 months ago
AI in Health care3 months agoAI in Medical Imaging: What is Coming Next
-

 AI in Health care1 month ago
AI in Health care1 month agoDigital X-ray vs. Film X-ray: Which is better?
-
 Diagnostic & Hospital Equipments1 month ago
Diagnostic & Hospital Equipments1 month agoDEXA Bone Density Scanning: What You Need to Know About Bone Health
-
 Diagnostic & Hospital Equipments4 weeks ago
Diagnostic & Hospital Equipments4 weeks agoPET Scan Machines: Understanding the Technology, and Usage
